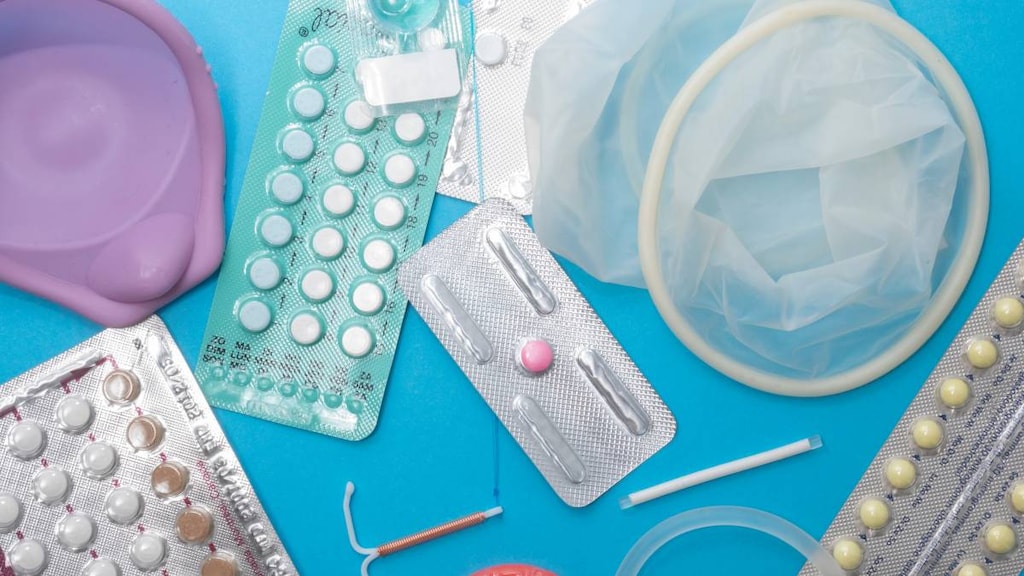
What is contraception?
Contraception is the deliberate use of a medicine, device, or a technique to prevent pregnancy that has the potential to happen during sexual intercourse. Contraception may also be called birth control.
A contraceptive is the name given to any medicine or device used for contraception.
What are contraceptives used For?
Contraceptives are mostly used for contraception (to help prevent women from becoming pregnant).
However, sometimes hormonal contraceptives may also be prescribed to:
- Help with acne control
- Help regulate periods
- Prevent ovulation and pregnancy in women with primary ovarian insufficiency (POI)
- Reduce pain and cramping during menstruation
- Reduce the symptoms of endometriosis, polycystic ovary syndrome (PCOS), premenstrual syndrome or premenstrual dysphoric disorder (PMDD).
Emergency contraceptives are contraceptives that are taken (or inserted if an IUD) within a few days after unprotected sex to help prevent implantation of a fertilized egg and possible resulting pregnancy.
Condoms are contraceptives that may be used to reduce the transmission of sexually transmitted infections, although protection is not 100%.
What are the differences between contraceptives?
There are several differences between contraceptives. The main difference is that some contain hormones whereas others do not. Hormone-containing contraceptives have more side effects than nonhormonal contraceptives. Some combined hormonal contraceptives also contain supplements such as iron or folic acid.
The following are different types of contraceptives:
- Combined oral contraceptives (COCs): These contain an estrogen and a progestin to prevent ovulation (the release of an egg from an ovary), thin the uterine lining, and thicken cervical mucus making it impenetrable to sperm
- Progestin-only contraceptives (POPs): These contain just one hormone, progestin. Most work by thickening cervical mucus, preventing sperm from entering the uterus. POPs must be taken within three hours of the same time every day
- Hormonal contraceptive patch: One patch is applied each week for every three weeks, then usually followed by a patch-free week
- Hormonal contraceptive rings: One ring is inserted into the vagina and remains in place continuously for three weeks, then removed for a one week break before a new ring is inserted
- Hormonal shot/injection: An injection is administered under the skin once every 3 months (12 to 14 weeks)
- Intrauterine devices (IUD): A small, T-shaped device that is inserted through the vagina into the uterus to prevent implantation of a fertilized egg. Lasts 3 to 10 years depending on the type
- Implantable rods: A small rod the size of a matchstick that is implanted under the skin of the upper arm. Lasts up to 3 years
- Female condom: Must be used every time that sex occurs. Provides some protection against STIs
- Male condom: Contain either latex, polyurethane, or polyisoprene. Must be used every time that sex occurs. Provide some protection against STIs
- Cervical cap/diaphragm with spermicide: A soft silicone cup that covers the cervix and is inserted before sex. May irritate, cause allergic reactions, and increase the risk of an abnormal Pap test
- Sponge with spermicide: Soft polyurethane sponge that is inserted before sex and kept in place for six hours after sex
- Spermicide alone: Must be used every time that sex occurs. Not very reliable. May irritate, cause allergic reactions, and increase the risk of STIs and UTIs.
Emergency hormonal contraception
The emergency contraceptive pill (ECP), sometimes called the ‘morning-after pill’ may be taken to prevent pregnancy after unprotected sex, contraceptive failure, or after a sexual assault.
Levonorgestrel ECPs work best if taken within 72 hours of unprotected sex; however, they are still moderately effective if used within five days of unprotected sex.
The ulipristal ECP can be used within five days of unprotected sex.
Is contraception safe?
Some types of contraception may not be suitable for some people.
Hormonal contraceptives are not recommended in women with certain types of cancer, at higher risk of clotting or strokes, with liver disease, severe headaches, undiagnosed vaginal bleeding, uncontrolled high blood pressure or heart disease. Nonhormonal methods of contraception are more suitable for these women.
Women who are pregnant who still wish to protect themselves from sexually transmitted infections should use barrier methods of contraception (such as condoms).
Serious side effects associated with hormonal contraceptives include:
- Blurred vision
- Chest pain and an increased risk of blood clots, heart attack, and stroke
- Leg pain or swelling
- A severe headache
- Severe stomach pain.
Smoking increases the risk of serious heart side effects with COCs (includes the hormonal ring or patch). COCs should NOT be used in women aged over 35 years who smoke because they are at higher risk of serious side effects such as heart attack, blood clots, or stroke.
Certain medications and some supplements can make hormonal contraceptives less effective. Hormonal contraceptives do not offer any protection against STIs such as HIV or hepatitis. Male or female condoms should be used in combination with hormonal contraceptives if protection against STIs is needed.
What are common side effects associated with contraception?
Hormonal contraceptives have been associated with several different side effects such as:
- Acne
- Appetite changes
- Breast tenderness, enlargement or discharge
- Changes to menstrual flow, bleeding or spotting between periods, painful or missed periods
- Constipation or diarrhea
- Gingivitis (inflammation of the gums)
- Hair growth in unusual places
- Mood changes
- Nausea
- Skin color changes (brown or black patches)
- Stomach cramps or bloating
- Weight gain or loss
- Vaginal burning, discharge, irritation, itching, redness, or swelling
- Vomiting.
Nonhormonal contraceptives may be associated with irritation, itching, redness, or discomfort during sex.




