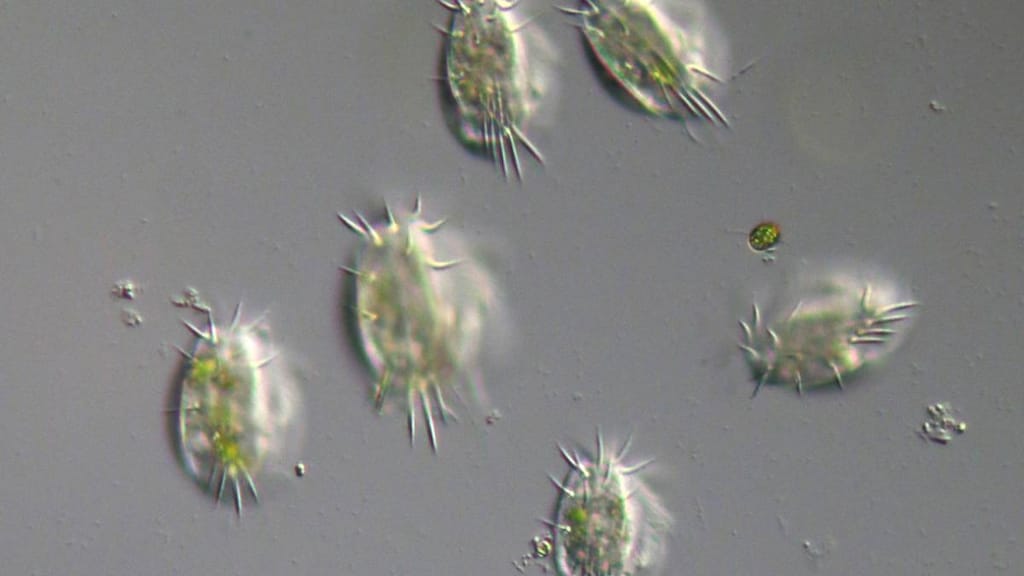
What is a protozoan infection?
Protozoan infections are infections caused by microscopic one-celled organisms that were formerly classified in the Kingdom Protozoa. This terminology is discouraged in the modern biosciences but still encountered in medicine. They are an extremely diverse and unique group.
Those that are infectious to humans may be classified into superclasses according to their mode of movement, for example:
- Sarcodina – the ameba (for example, Entamoeba). These move by changing their body shape, forming extensions called pseudopods (“false feet”)
- Mastigophora – the flagellates (for example, Giardia, Leishmania). These use flagella (slender, thread-like structures) like oars or to create waves to move
- Ciliophora – the ciliates (for example, Balantidium). These have hundreds of tiny cilia (minute hair-like projections) that beat in unison to propel them forwards or backward
- Sporozoa – these are immobile organisms (for example, Plasmodium, Cryptosporidium).
These organisms are free-living or parasitic. They are found worldwide in most habitats.
Infections range from symptomless to life-threatening depending on the species and strain of the parasite and the immunity of the host.
How are protozoan infections transmitted?
Protozoan infections are usually contracted by an insect vector or after contact with an infected substance or surface. For example:
- Protozoa that live in the human intestine are transmitted to other humans through the fecal-oral route (food, water, or other substances put in the mouth are contaminated with feces containing the protozoa)
- Protozoa that live in the blood or body tissues are transmitted to other humans through the bite of an insect, such as a mosquito or sand-fly, or another animal.
They readily multiply in humans, which means a serious infection can develop from just a single organism. This also increases their ability to survive and persist in the environment.
What are the symptoms of protozoan infections?
Protozoan infections are responsible for a wide range of different diseases that affect not only humans but animals and plants as well.
Symptoms vary depending on the type of infection, and many are deadly.
The following are a few examples of protozoan infections:
- African trypanosomiasis (African Sleeping Sickness)
- American trypanosomiasis (Chagas disease)
- Amoebiasis
- Leishmaniasis
- Toxoplasmosis.
African trypanosomiasis (African Sleeping Sickness)
Caused by the transmission of the protozoan parasite Trypanosoma brucei through the bite of a tsetse fly.
Initially, an itchy, painful, chancre (ulcer) forms at the site of the bite within 48 hours.
The resulting course of the disease has two distinct phases. Flu-like symptoms, limb swelling, enlarged lymph nodes, heart inflammation, disseminated intravascular coagulation, and kidney disease occur, followed by infection of the central nervous system when the parasites cross the blood-brain barrier. This results in drowsiness, nighttime insomnia, behavioral changes, mood disorders, headaches, and muscle disorders. Speech, gait, and reflexes are all affected.
American trypanosomiasis (Chagas disease)
Caused by the transmission of the protozoan parasite Trypanosoma cruzi via the triatomine bug (also known as kissing bugs). Parasites are deposited in the feces of the bug and enter via contact with mucosal surfaces or breaks in the skin. Parasites may also be transmitted during pregnancy, accidentally eating the bugs or the feces, or by blood transfusion or organ transplantation.
Many people have no symptoms or if they do, their symptoms resemble other common viral illnesses such as the flu so Chagas disease may go undetected. Newborns, children and those with impaired immunity may develop enlarged lymph nodes, heart inflammation, and enlarged liver or spleen. Chagomas (boil-like hardened, violet lesions with central swelling) may occur when the parasite has entered through a break in the skin. Eye swelling (known as the Romana sign) may form if the parasite entered via the conjunctiva. A short-lasting non-itchy skin rash that resembles measles may also develop. Left untreated Chagas can cause serious heart and gastrointestinal disease.
Amoebiasis
Caused by fecal-oral transmission of the protozoa, Entamoeba histolytica which is found worldwide. Diarrhea is the main symptom as most cases are confined to the intestines, although occasionally they can invade the mucosal wall or the bloodstream.
Leishmaniasis
Caused by the protozoa Leishmania, Leishmaniasis is transmitted by sandflies and is endemic in more than 70 countries worldwide. Symptoms vary depending on the infecting species, but the formation of a painless, usually solitary skin lesion of approximately 2cm with central ulceration that exudes pus or crusts over two weeks to six months after the initial bite is the most common presentation.
Toxoplasmosis
Caused by the protozoan parasite Toxoplasma gondii which is estimated to infect up to one-third of the world’s population. Humans can become infected through contact with cat feces, unwashed fruit or vegetables, by eating undercooked contaminated meat, organ donation or blood transfusion.
Symptoms include flu-like illness or eye inflammation (chorioretinitis). Rarely heart, brain or lung inflammation may occur. Skin lesions and rashes may occur. The infection may be life-threatening in people with impaired immunity.
How are protozoan infections diagnosed?
See your doctor if you suspect you have a protozoan infection. Your doctor will ask you about your travel history and possible contact with insects, animals, or contaminated food or water.
Several diagnostic blood tests are available that test for protozoan infections, but other tests (such as biopsies or stool samples) may be needed.
How are protozoan infections treated?
Treatment depends on the type of protozoan infection and the extent of the disease. Some medications are not registered in some countries. For example:
- African sleeping sickness: Suramin or pentamidine may be used if the parasite has not crossed the blood-brain barrier. Otherwise melarsoprol, nitrofurazone, or eflornithine
- Chagas disease: Antiparasitic treatment, such as nifurtimox or benznidazole. Supportive treatment such as pacemakers or antiarrhythmics
- Amebiasis: Medications such as iodoquinol, paromomycin, or diloxanide furoate
- Leishmaniasis: Treatments vary but may include cryotherapy, imiquimod, antifungals, and systemic antimonials
- Toxoplasmosis: Sulfadiazine with pyrimethamine or clindamycin.




