What is Rapamune?
- Rapamune is a prescription medicine used to prevent rejection (anti-rejection medicine) in people 13 years of age and older who have received a kidney transplant. Rejection is when your body's immune system recognizes the new organ as a "foreign" threat and attacks it.
Rapamune is used with other medicines called cyclosporine (Gengraf, Neoral, Sandimmune), and corticosteroids. Your doctor will decide:- if Rapamune is right for you, and
- how to best use it with cyclosporine and corticosteroids after your transplant.
- Rapamune is a prescription medicine also used to treat lymphangioleiomyomatosis (LAM). LAM is a rare progressive lung disease that affects predominantly women of childbearing age.
It is not known if Rapamune is safe and effective in children under 13 years of age.
What is the most important information I should know about Rapamune?
Rapamune can cause serious side effects, including:
- Increased risk of getting infections. Serious infections can happen including infections caused by viruses, bacteria, and fungi (yeast). Your doctor may put you on medicine to help prevent some of these infections.
Call your doctor right away if you have symptoms of infection including fever or chills while taking Rapamune. - Increased risk of getting certain cancers. People who take Rapamune have a higher risk of getting lymphoma, and other cancers, especially skin cancer. Talk with your doctor about your risk for cancer.
Rapamune has not been shown to be safe and effective in people who have had liver or lung transplants. Serious complications and death may happen in people who take Rapamune after a liver or lung transplant. You should not take Rapamune if you have had a liver or lung transplant without talking with your doctor.
See the section "What are the possible side effects of Rapamune?" for information about other side effects of Rapamune.
Who should not take Rapamune?
Do not take Rapamune if you are allergic to sirolimus or any of the other ingredients in Rapamune. See the end of this leaflet for a complete list of ingredients in Rapamune.
What should I tell my healthcare provider before taking Rapamune?
- have liver problems
- have skin cancer or it runs in your family
- have high cholesterol or triglycerides (fat in your blood)
- are pregnant or are a female who can become pregnant. Rapamune can harm your unborn baby. You should not become pregnant during treatment with Rapamune and for 12 weeks after ending treatment with Rapamune. In order to avoid pregnancy, a female who can get pregnant should use effective birth control during treatment and for 12 weeks after your final dose of Rapamune. Talk with your doctor about what birth control method is right for you during this time. Tell your doctor right away if you become pregnant or think you are pregnant during treatment with Rapamune or within 12 weeks after your final dose of Rapamune.
- It is not known whether Rapamune passes into breast milk; however, there is a risk of serious side effects in breastfed infants. You and your doctor should decide about the best way to feed your baby if you take Rapamune.
Tell your doctor about all the medicines you take, including prescription and over-the-counter medicines, vitamins and herbal supplements. Using Rapamune with certain medicines may affect each other causing serious side effects.
Rapamune may affect the way other medicines work, and other medicines may affect how Rapamune works.
Especially tell your doctor if you take:
- a medicine to lower your cholesterol or triglycerides
- cyclosporine (including Gengraf, Neoral, Sandimmune) or tacrolimus (Prograf) or other medicines that suppress the immune system
- an antibiotic
- an antifungal medicine
- a medicine for high blood pressure or heart problems
- an anti-seizure medicine
- medicines used to treat stomach acid, ulcers, or other gastrointestinal problems
- bromocriptine mesylate (Parlodel, Cycloset)
- danazol
- medicines to treat HIV or hepatitis C
- St. John's Wort
How should I take Rapamune?
- Read the Instructions for Use that comes with your Rapamune for information about the right way to take Rapamune oral solution.
- Take Rapamune exactly as your doctor tells you to take it.
- Your doctor will tell you how much Rapamune to take and when to take it. Do not change your dose of Rapamune unless your doctor tells you to.
- If you also take cyclosporine (Gengraf, Neoral, Sandimmune), you should take your Rapamune and cyclosporine about 4 hours apart.
- Do not stop taking Rapamune or your other anti-rejection medicines unless your doctor tells you to.
- Your doctor will check the levels of Rapamune in your blood. Your doctor may change your dose of Rapamune depending on your blood test results.
- Rapamune is taken by mouth 1 time each day.
- Do not crush, chew, or split Rapamune tablets. Tell your doctor if you cannot swallow Rapamune tablets. Your doctor can prescribe Rapamune as a solution.
- Take each dose of Rapamune the same way, either with or without food. Food can affect the amount of medicine that gets into your bloodstream. Taking each dose of Rapamune the same way helps keep your blood levels of Rapamune more stable. Do not take Rapamune with grapefruit juice.
- Rapamune oral solution can develop a slight haze when it is refrigerated. If this happens, bring the Rapamune Oral Solution to room temperature and then gently shake the bottle until the haze goes away.
- If you get Rapamune oral solution on your skin, wash the area with soap and water.
- If you get Rapamune oral solution in your eyes, rinse your eyes with water.
- If you have taken more medicine than you were told, contact a doctor or go to the nearest hospital emergency department right away.
What should I avoid while taking Rapamune?
- Avoid receiving live vaccines while taking Rapamune. Some vaccines may not work as well while you are taking Rapamune.
- Limit your time in sunlight and UV light. Cover your skin with clothing and use a broad spectrum sunscreen with a high protection factor because of the increased risk for skin cancer with Rapamune.
What are the possible side effects of Rapamune?
Rapamune may cause serious side effects, including:
- See "What is the most important information I should know about Rapamune?"
- Serious allergic reactions. Tell your doctor or get medical help right away if you get any of following symptoms of an allergic reaction:
- swelling of your face, eyes, or mouth
- trouble breathing or wheezing
- throat tightness
- chest pain or tightness
- feeling dizzy or faint
- rash or peeling of your skin
- Swelling (edema). Fluid may collect in your hands and feet and in various tissues of your body, including in the sac around your heart or lungs. Call your doctor if you have trouble breathing.
- Poor wound healing. Rapamune may cause your wounds to heal slowly or not heal well. Tell your doctor if you have any redness or drainage, your wound does not heal, or the wound opens up.
- Increased levels of cholesterol and triglycerides (lipids or fat) in your blood. Your doctor should do blood tests to check your lipids during treatment with Rapamune. Your doctor may prescribe treatment with diet, exercise, or medicine if your lipid levels are too high. During treatment with Rapamune, your blood levels of cholesterol and triglycerides may remain high even if you follow your prescribed treatment plan.
- Effects on kidney function. When Rapamune is taken with cyclosporine (Gengraf, Neoral, Sandimmune), the function of your transplanted kidney may be affected. Your doctor should regularly do tests to check your kidney function while you are taking Rapamune with cyclosporine (Gengraf, Neoral, Sandimmune).
- Increased protein in your urine. Your doctor may regularly test your urine protein.
- Increased risk for viral infections.
- Certain viruses can live in your body and cause active infections when your immune system is weak. BK virus can affect how your kidney works and cause your transplanted kidney to fail.
- A certain virus can cause a rare serious brain infection called Progressive Multifocal Leukoencephalopathy (PML). PML usually causes death or severe disability. Call your doctor right away if you notice any new or worsening medical problems such as:
- confusion
- sudden change in thinking, walking, strength on one side of your body
- other problems that have lasted over several days
- Lung or breathing problems. This can sometimes lead to death. Tell your doctor if you have a new or worsening cough, shortness of breath, difficulty breathing or any new breathing problems. Your doctor may need to stop Rapamune or lower your dose.
- Blood clotting problems. When Rapamune is taken with cyclosporine or tacrolimus, you may develop a blood clotting problem. Tell your doctor if you get any unexplained bleeding or bruising.
- Possible harm to your unborn baby. Rapamune can harm your unborn baby. You should not become pregnant during treatment with Rapamune and for 12 weeks after ending treatment with Rapamune. See "What should I tell my doctor before taking Rapamune?".
The most common side effects of Rapamune in people with renal transplant include:
- high blood pressure
- pain (including stomach and joint pain)
- diarrhea
- headache
- fever
- urinary tract infection
- low red blood cell count (anemia)
- nausea
- low platelet count (cells that help blood to clot)
- high blood sugar (diabetes)
The most common side effects of Rapamune in people with LAM include:
- mouth sores
- diarrhea
- stomach pain
- nausea
- sore throat
- acne
- chest pain
- upper respiratory tract infection
- headache
- dizziness
- sore muscles
Other side effects that may occur with Rapamune:
- Rapamune may affect fertility in females and may affect your ability to become pregnant. Talk to your healthcare provider if this is a concern for you.
- Rapamune may affect fertility in males and may affect your ability to father a child. Talk to your healthcare provider if this is a concern for you.
Tell your doctor if you have any side effect that bothers you or that does not go away.
These are not all of the possible side effects of Rapamune. For more information ask your doctor or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
Rapamune Images
General information about the safe and effective use of Rapamune
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use Rapamune for a condition for which it was not prescribed. Do not give Rapamune to other people even if they have the same symptoms that you have. It may harm them.
This Medication Guide summarizes the most important information about Rapamune. If you would like more information talk to your doctor. You can ask your pharmacist or doctor for information about Rapamune that is written for health professionals.
For more information, go to www.rapamune.com or call 1-800-934-5556.
How should I store Rapamune?
Rapamune tablets:
- Store Rapamune tablets at room temperature between 68°F to 77°F (20°C to 25°C).
- Blister cards and strips: Keep the tablets in the original blister container and use the outer carton to protect blister cards and strips from light.
- Bottles: Keep the bottle of Rapamune tablets tightly closed.
Rapamune oral solution:
- Store bottles of Rapamune oral solution in the refrigerator between 36°F to 46°F (2°C to 8°C).
- Protect from light.
- If necessary, bottles of Rapamune oral solution can be stored at room temperature up to 77°F (25°C) for up to 15 days.
- When a bottle of Rapamune oral solution is opened, it should be used within 1 month.
- Use any diluted Rapamune oral solution right away.
Do not use Rapamune after the expiration date. The expiration date refers to the last day of that month.
Safely throw away medicine that is out of date or no longer needed.
Keep Rapamune and all medicines out of the reach of children.
What are the ingredients in Rapamune?
Active ingredients: sirolimus
Inactive ingredients:
Oral Solution: Phosal 50 PG (phosphatidylcholine, propylene glycol, mono- and di-glycerides, ethanol, soy fatty acids, and ascorbyl palmitate) and polysorbate 80. Rapamune Oral Solution contains 1.5%–2.5% ethanol.
Tablets: sucrose, lactose, polyethylene glycol 8000, calcium sulfate, microcrystalline cellulose, pharmaceutical glaze, talc, titanium dioxide, magnesium stearate, povidone, poloxamer 188, polyethylene glycol 20,000, glyceryl monooleate, carnauba wax, dl-alpha tocopherol, and other ingredients. The 0.5 mg and 2 mg dosage strengths also contain yellow iron (ferric) oxide and brown iron (ferric) oxide.
Instructions for use for Rapamune
Rapamune /RAAP-a-mune/
(sirolimus)
Oral Solution
Be sure that you read and understand the following instructions for the correct way to dilute and take Rapamune Oral Solution. Ask your pharmacist or doctor if you are not sure.
Important:
- Always keep the bottle in an upright position.
- You may store Rapamune Oral Solution that is in a syringe at room temperature up to 77°F (25°C) or in the refrigerator at 36°F to 46°F (2°C to 8°C) for up to 24 hours. See "How should I store Rapamune?" at the end of this Instructions for Use.
- Rapamune Oral Solution can develop a slight haze when it is refrigerated. If this happens, bring the Rapamune Oral Solution to room temperature and then gently shake the bottle until the haze goes away.
- Only use a glass or plastic cup to dilute Rapamune Oral Solution.
- If you are a caregiver, do not let Rapamune Oral Solution come in contact with your skin or eyes. If you get the oral solution on your skin, wash the area well with soap and water. If you get the oral solution in your eyes, rinse with plain water.
- If you spill Rapamune Oral Solution, dry the area with a dry paper towel and then wipe the area with a wet paper towel. Throw away the paper towels in the trash and wash your hands well with soap and water.
Each Rapamune Oral Solution carton contains:
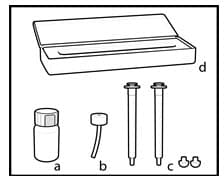
a) a 2 oz. (60 mL fill) amber glass bottle of sirolimus (concentration of 1 mg/mL)
b) 1 oral syringe adapter for fitting into the neck of the bottle
c). enough disposable oral syringes (amber color) and caps for daily dosing
d) 1 carrying case
You will also need:
- glass or plastic cup
- 6 oz. of water or orange juice only
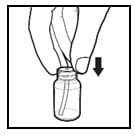
Figure 1: Opening the bottle
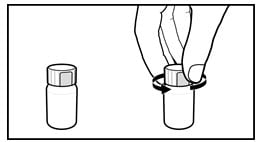
1. Open the solution bottle.
- Remove the safety cap by squeezing the tabs on each side of the cap and twisting counterclockwise (Figure 1).
Figure 2: Inserting adapter
2. The first time you use a bottle of Rapamune Oral Solution:
- Insert the oral syringe adapter (plastic tube with stopper) tightly into the bottle until it is even with the top of the bottle (Figure 2).
- Do not remove the oral syringe adapter from the bottle once inserted.
Figure 3: Inserting syringe
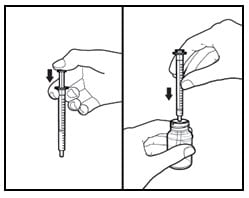
3. Use a new disposable amber oral syringe for each dose of Rapamune Oral Solution.
- Fully push down (depress) on the plunger of the disposable amber oral syringe.
- Then, tightly insert the oral syringe into the opening in the adapter (Figure 3).
Figure 4: Withdrawing solution
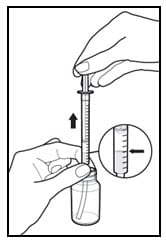
4. Withdraw the prescribed amount of Rapamune Oral Solution:
- Gently pull back the plunger of the syringe until the level of the oral solution is even with the marking on the syringe for your prescribed dose.
- Always keep the bottle in an upright position.
- If bubbles form within the oral solution in the syringe, empty the syringe into the bottle and repeat step 4 (Figure 4).
- You may need to repeat step 4 more than once to draw up your prescribed dose.
Figure 5: Capping syringe
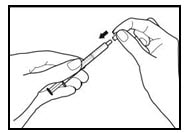
5. If your doctor tells you to carry your medicine with you:
- Each dose of Rapamune Oral Solution should be placed in an oral syringe. Place a cap securely on each syringe. The cap should snap into place (Figure 5).
- Place the capped syringe in the enclosed carrying case (Figure 6). If you need more than 1 carrying case, talk with your doctor or pharmacist.
- See 'How should I store Rapamune' for storage instructions.
Figure 6: Placing syringe in carrying case
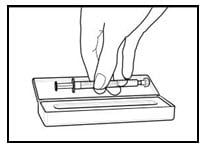
6. Place syringe in carrying case
Figure 7: Emptying syringe into glass
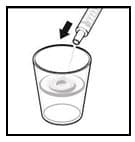
7. Taking a dose of Rapamune Oral Solution:
- Choose a clean flat work surface. Place a clean paper towel on the work surface. Wash and dry your hands.
- Empty the syringe into a glass or plastic cup containing at least 2 ounces (1/4 cup, 60 mL) of water or orange juice, stir vigorously for 1 minute and drink right away (Figure 7).
- If more than 1 syringe is needed for your prescribed dose, empty the oral solution from each syringe into the same glass or plastic cup of water or orange juice.
- Refill the container with at least 4 ounces (1/2 cup, 120 mL) of water or orange juice, stir vigorously again and drink the rinse solution. Do not mix Rapamune Oral Solution with apple juice, grapefruit juice, or other liquids. Only glass or plastic cups should be used to mix Rapamune Oral Solution.
- The syringe and cap should be used only one time and then thrown away.
- Throw away the paper towel and clean the work surface. Wash your hands.
8. Always store the bottles of medication in the refrigerator.
- Store bottles of Rapamune Oral Solution in the refrigerator at 36°F to 46°F (2°C to 8°C).
- Protect from light.
- Store Rapamune Oral Solution that is in a syringe at room temperature up to 77°F (25°C) or in the refrigerator at 36°F to 46°F (2°C to 8°C) for up to 24 hours.
- If necessary, bottles of Rapamune Oral Solution can be stored at room temperature up to 77°F (25°C) for up to 15 days.
- When a bottle of Rapamune Oral Solution is opened, it should be used within 1 month.
- Use any diluted Rapamune Oral Solution right away.
Keep Rapamune and all medicines out of the reach of children.
Instructions for use approved 06/2021.