10 Early Warning Signs of Prostate Cancer

Few cancer risks in men are as serious as prostate cancer. Other than skin cancer, no form of cancer is more common in men, according to the American Cancer Society. Among all men, about one in nine will develop the cancer at some point in their lives. In 2019, it’s estimated that nearly 175,000 American men will develop a new case of prostate cancer, and more than 30,000 men will die from prostate cancer.
However, prostate cancer is less likely to be deadly if it is detected and treated early. That makes it important for men to know the early warning signs of prostate cancer.
What you need to know about prostate cancer
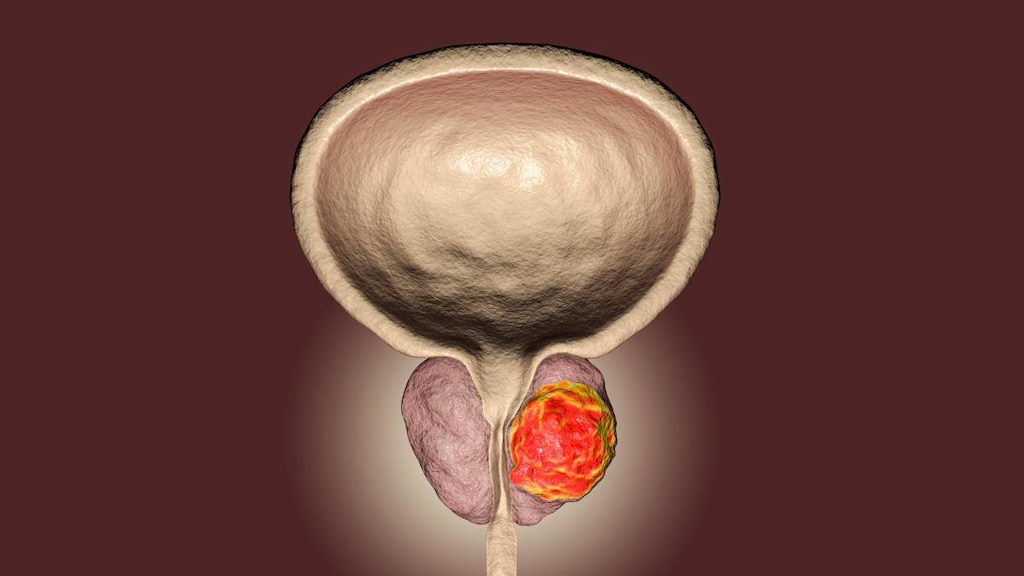
Unless it causes problems, most men don’t give a lot of thought to their prostate. The small gland is responsible for producing seminal fluid (fluid that helps sperm leave a man’s body after orgasm), and it’s located beneath the bladder and around the urethra, the tube that transports fluid to the penis.
Most types of prostate cancer are known as adenocarcinomas, which are cancers that develop from gland cells, the Mayo Clinic says.
While some forms of prostate cancer grow and spread quickly, others grow quite slowly. The American Cancer Society notes that some people can have undetectable prostate cancer for decades without it causing any problems. But the risks of prostate cancer are quite serious, particularly as it begins to spread to other areas of the body.
10 Warning signs of prostate cancer
One of the challenges of prostate cancer is that it often doesn’t present symptoms that alert men to its presence, particularly in the early stages. But the Urology Care Foundation notes that there may be some warning signs that you have problems related to your prostate, including the following:
- Frequent urge to urinate
- Weak or blocked urine flow
- Pain or burning while urinating
- Blood in the urine
- Painful ejaculation
- Pelvic pain
- Bone pain
- Hip, back or thigh pain
- Reduced appetite
- Weight loss
If you get screened for prostate cancer, there are additional warning signs based on how the prostate gland cells look under a microscope, notes the American Cancer Society. Cells that may be concerning will exhibit some level of what is known as prostatic intraepithelial neoplasia (PIN). These cells may exhibit low-grade PIN, in which something is slightly off with the cells, or high-grade PIN, when they show clear abnormalities.
Under a microscope, prostate gland cells may also exhibit what is known as proliferative inflammatory atrophy (PIA). PIA indicates cells that are smaller than normal and show some signs of inflammation. These cells may be worth additional monitoring because they could develop high-grade PIN and ultimately prostate cancer.
Risk factors for prostate cancer
Because prostate cancer tends to not show symptoms in its early stages, risk factors are another useful tool to identify candidates for screening. The Mayo Clinic notes that risk certainly increases as you grow older, and obese men may be more likely to have prostate cancer that is aggressive or difficult to treat.
For unknown reasons, black men are also at a greater risk of prostate cancer than men of other races. Not only are they more likely to get prostate cancer, but the risk of prostate cancer being aggressive or advanced is also higher.
Finally, your family history or genetics can also help determine your prostate cancer risk. For example, men with close relatives who had prostate cancer are more likely to get it. Also, a family history of breast cancer or the presence of the genes BRCA1 or BRCA2 within the family also raises the likelihood of a man developing prostate cancer.
When to see a doctor
Because it’s so difficult to identify prostate cancer early, it can often be difficult to know when it’s right to see the doctor. Of course, any of the warning signs and symptoms mentioned above warrant a trip to the doctor.
There are, however, other scenarios when you should see your doctor for prostate cancer screening, notes the Urology Care Foundation. For example, screening is generally recommended for men between the ages of 55 and 69. And if you have additional risk due to being African-American or having a family history of prostate cancer, then you may want to get screened earlier.
A wise approach: Talk to your doctor about whether prostate cancer screening would be right for you.
Diagnosing prostate cancer
Two primary tools are used in the frontline diagnosis of prostate cancer, according to the Mayo Clinic. The first is the prostate-specific antigen (PSA) test. This is a blood test in which the blood levels of PSA are determined. If a high amount is present, this may indicate some type of problem with the prostate — inflammation, an enlarged prostate, an infection or cancer.
When paired with a digital rectal exam, the PSA test can provide a better sense of the presence of prostate cancer. The exam involves manually inspecting the prostate through the rectum. The doctor will use a gloved, lubricated finger to do so. If both the digital rectal exam and the PSA test yield suspicious results, then additional testing may be needed.
Tests that can further confirm a prostate cancer diagnosis and help determine the treatment that is needed include ultrasound, performing a biopsy on a sample of tissue from the prostate and an imaging technology known as MRI fusion. Together, these tools can provide a clearer picture of the nature and extent of problems with the prostate.
Determining the proper treatment
There are a number of treatment options for prostate cancer, according to the Mayo Clinic.
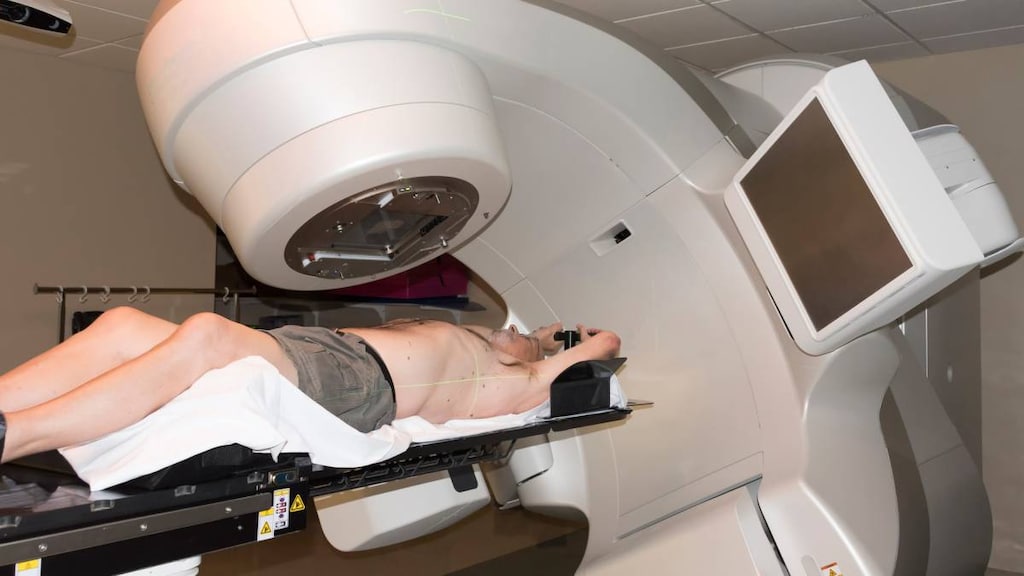
- Radiation. Radiation therapy can be delivered in a few different ways. One is external beam radiation, in which a machine outside the body delivers radiation to the prostate tissue. Another form of therapy, known as brachytherapy, involves using radioactive “seeds” to deliver a low dose of radiation directly to the prostate tissue.
- Hormones. The hormone testosterone acts as fuel for prostate cancer cells inside the body. By blocking the production of testosterone, you can kill off the cancer. Possible treatments include medications that stop the production of testosterone, medications that block testosterone from reaching cancer cells or, in extreme cases, surgery to remove the testicles.
- Surgery. For life-threatening prostate cancer, surgery to remove the prostate gland and surrounding tissues may be recommended.
- Biological therapy. Biological therapy uses your body’s own immune system to fight cancer. In the case of prostate cancer, your body’s immune cells are engineered in a lab to fight prostate cancer, and then injected back into your body.
- Chemotherapy. Chemotherapy is a traditional cancer treatment that’s used to stop its spread. It may be needed for prostate cancer that has spread to other areas of the body.
- Cryosurgery or cryoablation. Freezing prostate tissue and then thawing it out has shown some success in killing prostate cancer when other treatments have failed.
The bottom line
Prostate cancer is a risk that men need to be aware of, particularly as they grow older. By knowing the signs, symptoms and risk factors, men can work closely with their doctors and determine when screening is needed. Screening at the right time and in the appropriate circumstances may just catch prostate cancer early and save your life.
Article references
- Prostate Cancer, American Cancer Society, 2019, https://www.cancer.org/cancer/prostate-cancer.html
- Key Statistics for Prostate Cancer, American Cancer Society, 2019, https://www.cancer.org/cancer/prostate-cancer/about/key-statistics.html
- Prostate Cancer, Mayo Clinic, 2019, https://www.mayoclinic.org/diseases-conditions/prostate-cancer/diagnosis-treatment/drc-20353093
- What Is Prostate Cancer?, American Cancer Society, 2019, https://www.cancer.org/cancer/prostate-cancer/about/what-is-prostate-cancer.html
- What Is Prostate Cancer?, Urology Care Foundation, 2018, https://www.urologyhealth.org/urologic-conditions/prostate-cancer