Eye Allergies 101: Triggers & Treatment Options

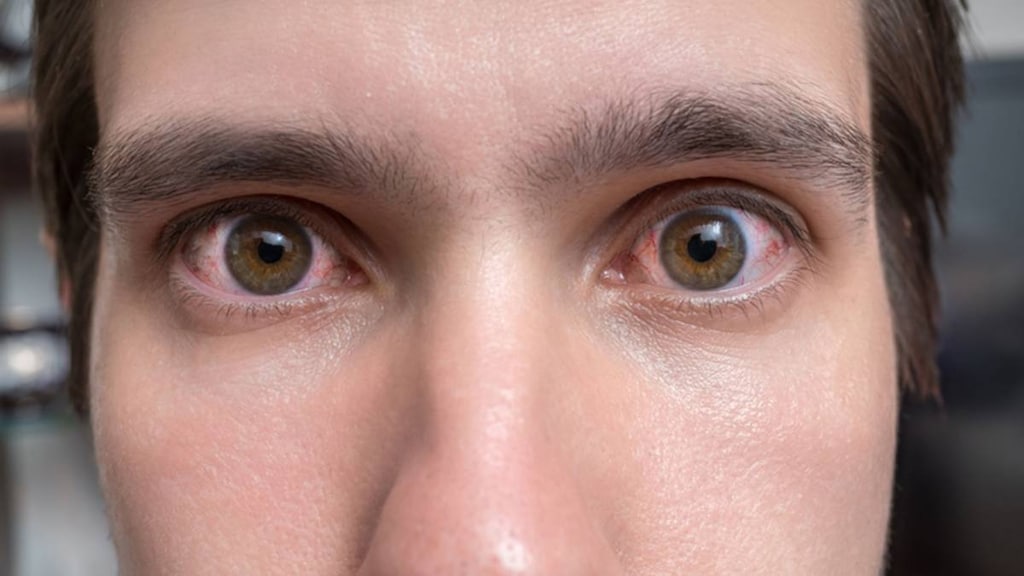
If you suffer from eyes that are watery, itchy, painful or red and swollen, you may be one of the millions of Americans who have an allergy that affects your eyes.
Eye allergies — known as allergic conjunctivitis or ocular allergy — occur when something irritates the delicate membrane covering the eye and the inside of the eyelid. When your immune system reacts to a usually harmless substance, that’s when an allergy begins. Once triggered, the immune system starts to make antibodies to that substance. Called Immunoglobulin E (IgE), these antibodies travel to the cells of the body, releasing chemicals that result in an allergic reaction, according to the American Academy of Ophthalmology.
When an allergic reaction affects your eyes, it inflames the conjunctiva, the mucous membrane covering the white of the eye and the inside of the eyelid.
What causes eye allergies?
Eye allergies are commonly caused by the same things that cause seasonal allergic reactions, like hay fever with its runny nose and sneezing. When pollen and mold spores are in the air, those symptoms get worse, especially when you’re outside when pollen counts are high.
Eyes are also vulnerable to indoor allergens such as dust mites and pet dander. Cleaning the house or grooming your dog or cat can make your symptoms worse.
Allergic reactions in the eyes can also be triggered by perfume, cosmetics or drugs. People can even be allergic to the preservative chemicals in some eye drops. The eyes can also react to other allergens that don’t come in direct contact with the eye. These can include some foods and insect bites and stings.
Eye allergies can also be inherited from your parents. If both your parents have eye allergies, then you’re more likely to have an allergy than if only one does, the American Academy of Ophthalmology says.
Symptoms and diagnosis
Eye allergies usually affect both eyes and can cause watery eyes, itchiness, sensitivity to light, redness, grittiness and swelling of the eyelid. These symptoms occur when small blood vessels widen and the eyes become pink or red. Some people have pain in one or both eyes, swollen eyelids, a burning sensation and sore or tender eyes. Symptoms can happen by themselves or be accompanied by sneezing and a runny nose and can start quickly after exposure to an allergen, according to the American Academy of Allergy, Asthma and Immunology.
Your best bet to get an accurate diagnosis is to see an allergist. Allergists are specially trained doctors who can find out what you’re allergic to and offer the best ways to treat your symptoms and avoid the things that trigger them. In addition to taking a full medical history, an allergist can test for the things that set off your allergic reactions.
Testing is usually done by pricking your skin with a sample of what you’re likely to be allergic to. It often takes about 20 minutes for a skin reaction that can confirm the allergy, but sometimes it takes longer. The doctor may also want to do a blood test and a conjunctival challenge test. This latter test is done by applying either dry or liquid materials that contain an allergen to one eye. The other eye gets a harmless substitute.
Avoiding triggers
One way to reduce the odds of an allergic reaction is to steer clear of those things that cause it. Simple steps that you can take, whether your allergy is to indoor or outdoor irritants like pollen and mold, include:
- Keeping your windows shut at night and using air conditioning, which cleans, cools and dries the air.
- Staying inside when pollen or mold counts are high. If you're outside, take a shower, shampoo your hair and change clothes when you get home.
- Not mowing lawns or raking leaves, which can stir up pollen and molds. And don’t hang clothes outside to dry.
- Keeping your car windows closed.
- Wearing a wide-brim hat and sunglasses to help reduce the amount of allergen that blows into the eyes.
- Using eye drops to rinse your eyes after being outdoors. This will help wash away allergens that get caught in your eyes.
Indoor allergens like dust or pet dander are harder to avoid, but you can keep these allergens down by using a vacuum with a HEPA filter to reduce dust and by keeping pets out of the bedroom, which will reduce the amount of dander you’re exposed to while you sleep.
Also, replace rugs and carpets — which trap and hold allergens — with hardwood, tile or other flooring materials that are easier to clean. And use window blinds instead of curtains that can store allergens. When cleaning floors, use a damp mop because sweeping can stir up allergens, making them easier to breathe in or get into your eyes.
To keep mold from growing in your home, keep the humidity under 50 percent. You can also use a dehumidifier. Be sure to clean the dehumidifier regularly. Also use bleach when you wash the kitchen and bathrooms, the American Academy of Allergy, Asthma and Immunology notes.
Another step you can take is to wear glasses instead of contact lenses, which can attract and accumulate allergens. If you really must use contacts, then switch to single-use disposable contacts. These will help avoid allergen buildup on the lenses. The best advice is to give up on contact lenses altogether, at least while your allergy symptoms persist. Eyeglasses with photochromic lenses can help reduce sensitivity to light caused by allergies and help shield your eyes from allergens in the air, according to the American Academy of Ophthalmology.
Treatment and relief
Fortunately, the symptoms of eye allergies won’t damage your vision, although they may cause temporary blurriness. Also, allergic conjunctivitis is not contagious like pink eye.
For short-term relief, over-the-counter antihistamine pills and eye drops can relieve symptoms. But using some eye drops may make your symptoms worse. An allergist can often prescribe stronger drugs if your symptoms are long-lasting, the Asthma and Allergy Foundation of America, says.
Among other treatments, eye drops containing corticosteroids can be effective but can also have side effects even when only used for a limited time. Corticosteroid eye drops should only be used under the direction of an ophthalmologist because side effects can include an increased risk of glaucoma, cataracts and infection.
Additional treatment can include allergy shots and other immunotherapies. These treatments can be long-lasting, depending on what you’re allergic to. Immunotherapy works by desensitizing the immune system to specific allergens that trigger symptoms in the first place.
Prescription eye drops and oral medications include:
- Antihistamines: Part of the body’s allergic response is to make histamine, which dilates blood vessels and makes their walls abnormally easy to breach. This is what causes a runny nose and itchy, watery eyes. Antihistamines block histamine from entering cells in the body that produce these allergic responses.
- Decongestants: Decongestants work by helping shrink swollen nasal passages for easier breathing and also reduce the size of blood vessels in the white of the eyes to relieve redness.
- Mast cell stabilizers: These drugs change cells that contain histamine, including in the conjunctiva of the eye and eyelids, thus preventing them from releasing histamine and thereby reducing allergic reactions. Because it may take several weeks before mast cell stabilizers become fully effective, these drugs are best when used before allergy season starts as a way to prevent or reduce the severity of allergic reactions before they begin.
- Non-steroidal anti-inflammatory drugs (NSAIDs): These eye drops can decrease swelling, inflammation and other symptoms tied to allergic conjunctivitis.
Article references
- What Are Eye Allergies? American Academy of Ophthalmology. https://www.aao.org/eye-health/diseases/allergies
- Eye Allergy: Symptoms and Diagnosis, American Academy of Allergy, Asthma and Immunology. https://www.aaaai.org/conditions-and-treatments/allergies/eye-allergy
- What Causes Eye Allergies? Asthma and Allergy Foundation of America. https://www.aafa.org/eye-allergy-conjunctivitis/