Hepatocellular carcinoma (HCC) is the most common type of primary liver cancer. Hepatocellular carcinoma occurs most often in people with chronic liver diseases, such as cirrhosis caused by hepatitis B or hepatitis C infection.
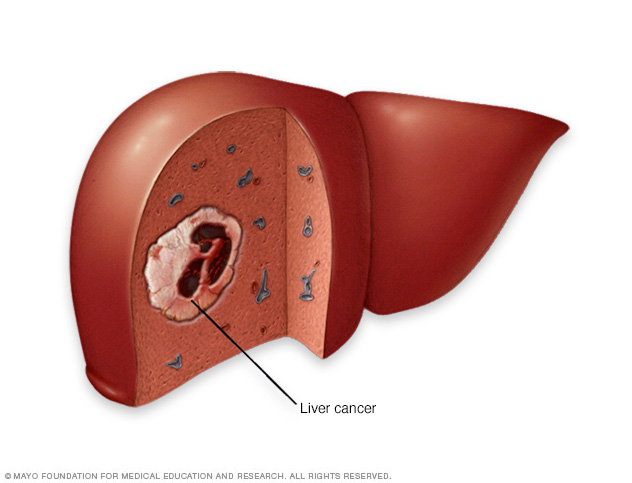
Liver cancer begins in the cells of the liver. The most common form of liver cancer begins in cells called hepatocytes and is called hepatocellular carcinoma.
Risk factors
The risk of hepatocellular carcinoma, the most common type of liver cancer, is higher in people with long-term liver diseases. It's also higher if the liver is scarred by infection with hepatitis B or hepatitis C. Hepatocellular carcinoma is more common in people who drink large amounts of alcohol and who have an accumulation of fat in the liver.
Diagnosis
Tests and procedures used to diagnose hepatocellular carcinoma include:
- Blood tests to measure liver function
- Imaging tests, such as CT and MRI
- Liver biopsy, in some cases, to remove a sample of liver tissue for laboratory testing
Treatment
Which treatment is best for you will depend on the size and location of your hepatocellular carcinoma, how well your liver is functioning, and your overall health.
Hepatocellular carcinoma treatments include:
- Surgery. Surgery to remove the cancer and a margin of healthy tissue that surrounds it may be an option for people with early-stage liver cancers who have normal liver function.
- Liver transplant surgery. Surgery to remove the entire liver and replace it with a liver from a donor may be an option in otherwise healthy people whose liver cancer hasn't spread beyond the liver.
- Destroying cancer cells with heat or cold. Ablation procedures to kill the cancer cells in the liver using extreme heat or cold may be recommended for people who can't undergo surgery. These procedures include radiofrequency ablation, cryoablation, and ablation using alcohol or microwaves.
- Delivering chemotherapy or radiation directly to cancer cells. Using a catheter that's passed through your blood vessels and into your liver, doctors can deliver chemotherapy drugs (chemoembolization) or tiny glass spheres containing radiation (radioembolization) directly to the cancer cells.
- Radiation therapy. Radiation therapy using energy from X-rays or protons may be recommended if surgery isn't an option. A specialized type of radiation therapy, called stereotactic body radiotherapy (SBRT), involves focusing many beams of radiation simultaneously at one point in your body.
- Targeted drug therapy. Targeted drugs attack specific weaknesses in the cancer cells, and they may help slow the progression of the disease in people with advanced liver cancers.
- Immunotherapy. Immunotherapy drugs use your body's germ-fighting immune system to attack the cancer cells. Immunotherapy may be an option for treating advanced liver cancer.
- Clinical trials. Clinical trials give you a chance to try new liver cancer treatments. Ask your doctor whether you're eligible to participate in a clinical trial.
Copyright © 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved.