Hyperparathyroidism is when your parathyroid glands create high amounts of parathyroid hormone in the bloodstream. These glands, located behind the thyroid at the bottom of your neck, are about the size of a grain of rice.
The parathyroid hormone produced by the thyroid glands helps maintain the right balance of calcium in the bloodstream and in tissues that depend on calcium for proper functioning. This is especially important for nerve and muscle function, as well as bone health.
There are two types of hyperparathyroidism. In primary hyperparathyroidism, an enlargement of one or more of the parathyroid glands causes overproduction of parathyroid hormone. This causes high calcium levels in the blood, which can cause a variety of health problems. Surgery is the most common treatment for primary hyperparathyroidism.
Secondary hyperparathyroidism occurs due to another disease that first causes low calcium levels in the body. Over time, increased parathyroid hormone levels occur as the body fights to keep the calcium level up in the standard range. This is common in kidney disease and after certain intestinal surgeries or diseases.
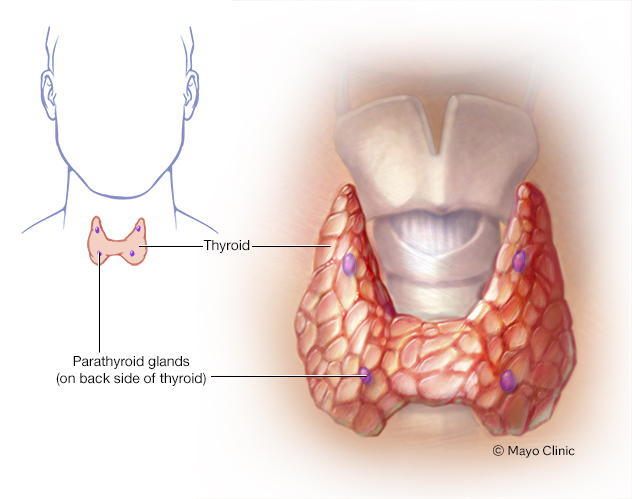
The parathyroid glands lie behind the thyroid. They produce parathyroid hormone, which plays a role in regulating the body's blood level of calcium and phosphorus.
Symptoms
Primary hyperparathyroidism is often diagnosed before signs or symptoms of the disorder occur. This is usually because an elevated level of calcium is found on routine blood tests. When symptoms do occur, they're the result of damage or dysfunction in other organs or tissues. This damage or dysfunction is due to high calcium levels in the blood and urine or too little calcium in bones.
Symptoms may be so mild and nonspecific that they don't seem related to parathyroid function, or they may be severe. The range of signs and symptoms include:
- Weak bones that break easily (osteoporosis)
- Kidney stones
- Excessive urination
- Stomach (abdominal) pain
- Tiring easily or weakness
- Depression or forgetfulness
- Bone and joint pain
- Frequent complaints of illness with no clear cause
- Nausea, vomiting or loss of appetite
When to see a doctor
See your health care provider if you have any signs or symptoms of hyperparathyroidism. These symptoms could be caused by many disorders, including some with serious complications. It's important to get a prompt, accurate diagnosis and the right treatment.
Causes
Hyperparathyroidism is caused by factors that increase the production of parathyroid hormone.
The parathyroid glands keep proper levels of both calcium and phosphorus in your body by turning the release of parathyroid hormone off or on. This is similar to how a thermostat controls a heating system to maintain a constant air temperature. Vitamin D also is involved in controlling the amount of calcium in your blood.
Normally, this balancing act works well.
- When calcium levels in your blood fall too low, your parathyroid glands release enough parathyroid hormone to restore the balance. This hormone raises calcium levels by releasing calcium from your bones, increasing the amount of calcium absorbed from your small intestine and decreasing the amount of calcium lost in urine.
- When blood-calcium levels are too high, the parathyroid glands produce less parathyroid hormone.
Calcium is best known for its role in keeping your teeth and bones healthy. But calcium also aids in the transmission of signals in nerve cells. And it's involved in muscle contraction. Phosphorus, another mineral, works along with calcium in these areas.
Sometimes one or more of the parathyroid glands produce high amounts of parathyroid hormone. These high hormone levels can be the body responding appropriately to keep the calcium in the standard range, or they may be inappropriately elevating the calcium in the blood. Which one depends on the underlying problem.
Hyperparathyroidism may occur because of primary hyperparathyroidism or secondary hyperparathyroidism.
Primary hyperparathyroidism
Primary hyperparathyroidism occurs because of a problem with one or more of the four parathyroid glands:
- A noncancerous growth (adenoma) on a gland is the most common cause.
- Enlargement (hyperplasia) of two or more parathyroid glands accounts for most other cases.
- A cancerous tumor is a very rare cause of primary hyperparathyroidism.
One or more of the parathyroid glands produces high amounts of parathyroid hormone. This leads to high calcium levels and low phosphorus levels in your blood. Primary hyperparathyroidism usually occurs randomly. But some people inherit a gene that causes the disorder.
Secondary hyperparathyroidism
Secondary hyperparathyroidism is the result of another condition that lowers the blood calcium, which then affects the gland's function. This causes your parathyroid glands to overwork and produce high amounts of parathyroid hormone to maintain or restore the calcium level to the standard range. Factors that may result in secondary hyperparathyroidism include:
- Severe calcium deficiency. Your body may not get enough calcium from your diet, often because your digestive system doesn't absorb the calcium from food. This is common after intestinal surgery, including weight loss surgery.
Severe vitamin D deficiency. Vitamin D helps maintain appropriate calcium levels in the blood. It also helps your digestive system absorb calcium from your food.
Your body produces vitamin D when your skin is exposed to sunlight. You also get some vitamin D in food. If you don't get enough vitamin D, then calcium levels may drop.
Chronic kidney failure. Your kidneys convert vitamin D into a form that your body can use. If your kidneys work poorly, usable vitamin D may decrease and calcium levels drop. This causes parathyroid hormone levels to go up. Chronic kidney failure is the most common cause of secondary hyperparathyroidism.
In some people with long-term secondary hyperparathyroidism, usually from end-stage kidney disease, the parathyroid glands enlarge. They begin to release parathyroid hormone on their own. The hormone level doesn't go down with medical treatment and the blood calcium becomes too high. This is called tertiary hyperparathyroidism, and people with this condition may require surgery to remove parathyroid tissue.
Risk factors
You may be at an increased risk of primary hyperparathyroidism if you:
- Are a woman who has gone through menopause
- Have had prolonged, severe calcium or vitamin D deficiency
- Have a rare, inherited disorder, such as multiple endocrine neoplasia, type 1, which usually affects multiple glands
- Have had radiation treatment for cancer that has exposed your neck to radiation
- Have taken lithium, a drug most often used to treat bipolar disorder
Complications
Complications of hyperparathyroidism are mainly related to the long-term effect of too little calcium in your bones and too much calcium in your bloodstream. Common complications include:
- Osteoporosis. The loss of calcium from bones often results in weak, brittle bones that break easily (osteoporosis).
- Kidney stones. Too much calcium in your blood may lead to too much calcium in your urine. This can cause small, hard deposits of calcium and other substances to form in your kidneys (kidney stone). A kidney stone usually causes major pain as it passes from the kidneys through the urinary tract.
- Cardiovascular disease. Although the exact cause-and-effect link is unclear, high calcium levels are associated with heart and blood vessel (cardiovascular) conditions, such as high blood pressure and certain types of heart disease.
- Neonatal hypoparathyroidism. Severe, untreated hyperparathyroidism in pregnant women may cause dangerously low levels of calcium in newborns. Primary hyperparathyroidism is not common in women of childbearing age.
Diagnosis
In most cases, elevated calcium is found by blood tests ordered for other reasons. For example, routine blood work or testing to figure out the cause of symptoms of another condition. Your provider may diagnose hyperparathyroidism by ordering:
Blood tests
If blood test results show that you have high calcium levels in your blood, your health care provider will likely repeat the test. This repeated test can confirm the results after you haven't eaten for a period of time.
Many conditions can raise calcium levels. But your health care provider can diagnose hyperparathyroidism if blood tests show you also have high levels of parathyroid hormone.
Additional tests
After diagnosing primary hyperparathyroidism, your health care provider will likely order more tests. These can rule out possible conditions causing hyperparathyroidism, identify possible complications and determine the severity of the condition. These tests include:
Bone mineral density test. This test is done to see if you have developed osteoporosis. The most common test to measure bone mineral density is dual-energy X-ray absorptiometry (DEXA).
This test uses special X-ray devices to measure how many grams of calcium and other bone minerals are packed into a bone segment.
Urine test. A 24-hour collection of urine can provide information on how well your kidneys work and how much calcium is passed in your urine.
This test may help your provider determine the severity of hyperparathyroidism or diagnose a kidney disorder causing hyperparathyroidism. If a very low calcium level is found in the urine, this may mean it's a condition that doesn't need treatment.
- Imaging tests of kidneys. Your provider may order an X-ray or other imaging tests of your abdomen to determine if you have kidney stones or other kidney problems.
Imaging tests before surgery
If your health care provider recommends surgery, one of these imaging tests may be used to locate the parathyroid gland or glands that are causing problems:
Sestamibi parathyroid scan. Sestamibi is a radioactive compound that is absorbed by overactive parathyroid glands. It can be detected by a scanner that detects radioactivity.
A healthy thyroid gland also absorbs sestamibi. To keep the thyroid absorption from blocking the view of the absorption in a parathyroid tumor (adenoma), you're also given radioactive iodine. This is only absorbed by the thyroid. Using this process, the thyroid image is digitally removed so it can't be seen.
Computerized tomography (CT) scanning may be combined with the sestamibi scan to improve detection of any problems with the parathyroid glands.
Ultrasound. Ultrasound uses sound waves to create images of your parathyroid glands and surrounding tissue.
A small device held against your skin (transducer) sends out high-pitched sound waves and records the sound wave echoes as they reflect off internal structures. A computer converts the echoes into images on a monitor.
Treatment
Treatment options for primary hyperparathyroidism can include watchful waiting, surgery and medications.
Watchful waiting
Your health care provider may recommend no treatment and regular monitoring if:
- Your calcium levels are only slightly elevated
- Your kidneys are working well, and you have no kidney stones
- Your bone density is within the standard range or only slightly below the range
- You have no other symptoms that may improve with treatment
If you choose this watch-and-wait approach, you'll likely need regularly scheduled tests to monitor your blood-calcium levels and bone density.
Surgery
Surgery is the most common treatment for primary hyperparathyroidism and provides a cure in most cases. A surgeon will remove only those glands that are enlarged or have a tumor.
If all four glands are affected, a surgeon will likely remove only three glands and perhaps a portion of the fourth — leaving some functioning parathyroid tissue.
Surgery may be done as an outpatient procedure, allowing you to go home the same day. In such cases, the surgery can be done through very small cuts (incisions) in the neck. You receive only local anesthetics to numb the area.
Complications from surgery aren't common. Risks include:
- Damage to nerves controlling the vocal cords.
- Long-term low calcium levels requiring the use of calcium and vitamin D supplements due to removal or damage to all parathyroid glands. This means the body cannot produce enough parathyroid hormone to keep the calcium in the standard range.
Medications
Medications to treat hyperparathyroidism include the following:
Calcimimetics. A calcimimetic is a drug that mimics calcium circulating in the blood. The drug may trick the parathyroid glands into releasing less parathyroid hormone. This drug is sold as cinacalcet (Sensipar).
Cinacalcet may be an option to treat primary hyperparathyroidism, particularly if surgery hasn't successfully cured the disorder or a person isn't a good surgery candidate.
Cinacalcet and vitamin D analogs (prescription forms of vitamin D) are used to manage secondary hyperparathyroidism in chronic kidney disease. These medications help keep the balance of calcium and phosphorus minerals so that the parathyroid glands don't have to work hard.
The most commonly reported side effects of cinacalcet are joint and muscle pain, diarrhea, nausea, and respiratory infection.
Hormone replacement therapy. For women who have gone through menopause and have signs of osteoporosis, hormone replacement therapy may help bones keep calcium. However, this treatment doesn't address the underlying problems with the parathyroid glands.
Prolonged use of hormone replacement therapy can increase the risk of blood clots and breast cancer. Work with your health care provider to evaluate the risks and benefits to help you decide what's best for you.
Some common side effects of hormone replacement therapy include breast pain and tenderness, dizziness, and headaches.
- Bisphosphonates. Bisphosphonates also prevent the loss of calcium from bones and may lessen osteoporosis caused by hyperparathyroidism. Some side effects associated with bisphosphonates include low blood pressure, a fever and vomiting. This treatment doesn't address the underlying problems with the parathyroid glands, and the blood calcium level remains above the standard range.
Lifestyle and home remedies
If you and your health care provider have chosen to monitor, rather than treat, your primary hyperparathyroidism, the following suggestions can help prevent complications:
Monitor how much calcium and vitamin D you get in your diet. Restricting how much calcium you eat or drink is not recommended for people with hyperparathyroidism.
The daily recommended amount of calcium for adults ages 19 to 50 and men ages 51 to 70 is 1,000 milligrams (mg) of calcium a day. That calcium recommendation increases to 1,200 mg a day for women age 51 and older and men age 71 and older.
The daily recommended amount of vitamin D is 600 international units (IUs) of vitamin D a day for people ages 1 to 70 and 800 IUs a day for adults age 71 and older. Talk to your provider about dietary guidelines that are right for you.
- Drink plenty of fluids. Drink enough fluids, mostly water, to produce nearly clear urine to lessen the risk of kidney stones.
- Exercise regularly. Regular exercise, including strength training, helps maintain strong bones. Talk to your provider about what type of exercise program is best for you.
- Don't smoke. Smoking may increase bone loss as well as increase your risk of several serious health problems. Talk to your provider about the best ways to quit.
- Avoid calcium-raising medications. Certain medications, including some diuretics and lithium, can raise calcium levels. If you take such medications, ask your provider whether another medication may be appropriate for you.
Preparing for an appointment
In most cases, elevated calcium is detected by blood tests your health care provider has ordered as part of a routine screening, tests for an unrelated condition or tests to identify the cause of very general symptoms.
Talk to your provider about your test results if they show you have high levels of calcium. Questions you might ask include:
- Do I have hyperparathyroidism?
- What test do I need to confirm the diagnosis or determine the cause?
- Should I see a specialist in hormone disorders (endocrinologist)?
- If I have hyperparathyroidism, do you recommend surgery?
- What alternatives do I have to surgery?
- I have these other health conditions. How can I best manage them together?
- Do you have printed material about hyperparathyroidism that I can take home?
To understand the effect of hyperparathyroidism on your overall health, your provider may ask you questions about possible mild signs or symptoms, including:
- Have you been feeling depressed?
- Do you often feel tired, easily fatigued or generally unwell?
- Are you feeling any unexplained aches and pains?
- Are you often forgetful, absent-minded or unable to concentrate?
- Have you experienced increased thirst and excessive urination?
Your health care provider may ask you additional questions about what medications you're taking and what your diet is like to help determine if you get adequate amounts of calcium and vitamin D.
Copyright © 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved.