What is ethinyl estradiol and norelgestromin transdermal system?
Ethinyl estradiol and norelgestromin transdermal system is a birth control patch for women with a BMI less than 30 kg/m2. It contains two female hormones, an estrogen called ethinyl estradiol, and a progestin called norelgestromin.
Hormones from ethinyl estradiol and norelgestromin transdermal system get into the blood stream and are processed by the body differently than hormones from birth control pills. You will be exposed to about 60% more estrogen if you use ethinyl estradiol and norelgestromin transdermal system than if you use a typical birth control pill containing 35 micrograms of estrogen. In general, increased estrogen may increase the risk of side effects.
How well does ethinyl estradiol and norelgestromin transdermal system work?
Your chance of getting pregnant depends on how well you follow the directions for using ethinyl estradiol and norelgestromin transdermal system. The better you follow the directions, the less chance you have of getting pregnant.
In clinical studies, 1 to 2 out of 100 women got pregnant during the first year that they used the norelgestromin and ethinyl estradiol transdermal system.
Ethinyl estradiol and norelgestromin transdermal system may not be as effective in women weighing more than 198 lbs. (90 kg). If you weigh more than 198 lbs. (90 kg), talk to your healthcare provider about which method of birth control is right for you.
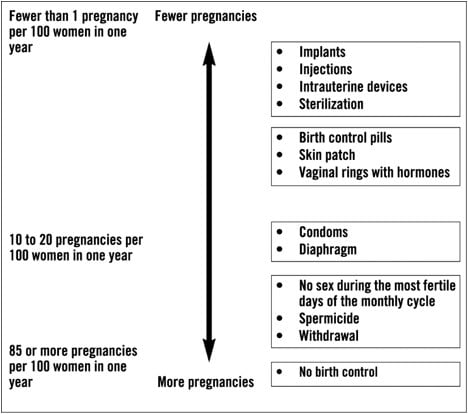
The following chart shows the chance of getting pregnant for women who use different methods of birth control. Each box on the chart contains a list of birth control methods that are similar in effectiveness. The most effective methods are at the top of the chart. The box on the bottom of the chart shows the chance of getting pregnant for women who do not use birth control and are trying to get pregnant.
Do hormonal birth control methods cause cancer?
Hormonal birth control methods do not seem to cause breast cancer. However, if you have breast cancer now, or have had it in the past, do not use hormonal birth control methods because some breast cancers are sensitive to hormones.
Women who use hormonal birth control methods may have a slightly higher chance of getting cervical cancer. However, this may be due to other reasons such as having more sexual partners.
What should I know about my period when using ethinyl estradiol and norelgestromin transdermal system?
When you use ethinyl estradiol and norelgestromin transdermal system you may have bleeding and spotting between periods, called unplanned bleeding. Unplanned bleeding may vary from slight staining between menstrual periods to breakthrough bleeding which is a flow much like a regular period. Unplanned bleeding occurs most often during the first few months of ethinyl estradiol and norelgestromin transdermal system use, but may also occur after you have been using the patch for some time. Such bleeding may be temporary and usually does not indicate any serious problems. It is important to continue using the patch on schedule. If the unplanned bleeding or spotting is heavy or lasts for more than a few days, you should discuss this with your healthcare provider.
What if I miss my scheduled period when using ethinyl estradiol and norelgestromin transdermal system?
Some women miss periods on hormonal birth control, even when they are not pregnant. However, if you go 2 or more months in a row without a period, or you miss your period after a month where you did not use all of your patches correctly, or you have symptoms associated with pregnancy, such as morning sickness or unusual breast tenderness, call your healthcare provider because you may be pregnant. Stop taking ethinyl estradiol and norelgestromin transdermal system if you are pregnant.
What if I want to become pregnant?
You may stop using ethinyl estradiol and norelgestromin transdermal system whenever you wish. Consider a visit with your healthcare provider for a pre-pregnancy checkup before you stop using the patch.
What is the most important information I should know about ethinyl estradiol and norelgestromin transdermal system?
Do not use ethinyl estradiol and norelgestromin transdermal system if you smoke cigarettes and are over 35 years old. Smoking increases your risk of serious cardiovascular side effects from hormonal birth control methods, including death from heart attack, blood clots or stroke. This risk increases with age and the number of cigarettes you smoke.
Do not use ethinyl estradiol and norelgestromin transdermal system if you have an increased risk for blood clots.
Do not use ethinyl estradiol and norelgestromin transdermal system if your Body Mass Index (BMI) is 30 kg/m2 or more. Women with a BMI of 30+ kg/m2 or more who use ethinyl estradiol and norelgestromin transdermal system may be at a higher risk for developing blood clots compared to women with a BMI lower than 30 kg/m2.
Hormonal birth control methods help to lower the chances of becoming pregnant. They do not protect against HIV infection (AIDS) and other sexually transmitted infections.
Who should not use ethinyl estradiol and norelgestromin transdermal system?
Do not use ethinyl estradiol and norelgestromin transdermal system if you:
- smoke and are over 35 years old
- have or have had blood clots in your arms, legs, eyes or lungs
- have an inherited problem that makes your blood clot more than normal
- have had a stroke
- have had a heart attack
- have certain heart valve problems or heart rhythm problems that can cause blood clots to form in the heart
- have high blood pressure that medicine cannot control
- have diabetes with kidney, eye, nerve, or blood vessel damage
- have had certain kinds of severe migraine headaches with aura, numbness, weakness or changes in vision, or have any migraine headaches if you are over age 35
- have liver disease, including liver tumors, take any Hepatitis C drug combination containing ombitasvir/paritaprevir/ritonavir, with or without dasabuvir. This may increase levels of the liver enzyme “alanine aminotransferase” (ALT) in the blood.
- have unexplained vaginal bleeding
- are pregnant or think you may be pregnant. However, ethinyl estradiol and norelgestromin transdermal system is not known to cause birth defects when used by accident during pregnancy.
- have had breast cancer or any cancer that is sensitive to female hormones
Hormonal birth control methods may not be a good choice for you if you have ever had jaundice (yellowing of the skin or eyes) caused by pregnancy or related to previous use of hormonal birth control.
Tell your healthcare provider if you have ever had any of the above conditions. Your healthcare provider may recommend another method of birth control.
What should I tell my healthcare provider before using ethinyl estradiol and norelgestromin transdermal system?
Before you use ethinyl estradiol and norelgestromin transdermal system tell your healthcare provider:
- about all your medical conditions
- if you are pregnant or think you are pregnant
- if you are scheduled for surgery. Ethinyl estradiol and norelgestromin transdermal system may increase your risk of blood clots after surgery. You should stop using your ethinyl estradiol and norelgestromin transdermal system patch at least 4 weeks before you have surgery and not restart it until at least 2 weeks after your surgery.
- if you are scheduled for any laboratory tests. Certain blood tests may be affected by hormonal birth control methods.
- are breastfeeding or plan to breastfeed. Hormonal birth control methods that contain estrogen, like ethinyl estradiol and norelgestromin transdermal system, may decrease the amount of milk you make. A small amount of hormones from the ethinyl estradiol and norelgestromin transdermal system patch may pass into your breast milk. Consider another method of birth control until you are ready to stop breastfeeding.
Tell your healthcare provider about all medicines and herbal products that you take.
Some medicines and herbal products may make hormonal birth control less effective, including, but not limited to:
- certain seizure medicines (carbamazepine, felbamate, oxcarbazepine, phenytoin, rufinamide, and topiramate)
- aprepitant
- barbiturates
- bosentan
- griseofulvin
- certain combinations of HIV medicines (nelfinavir, ritonavir, ritonavir-boosted protease inhibitors)
- certain non-nucleoside reverse transcriptase inhibitors (nevirapine)
- rifampin and rifabutin
- St. John’s wort
Use another birth control method (such as a condom and spermicide or diaphragm and spermicide) when you take medicines that may make the ethinyl estradiol and norelgestromin transdermal system patch less effective.
Some medicines and grapefruit juice may increase your level of the hormone ethinyl estradiol if used together, including:
- acetaminophen
- ascorbic acid
- medicines that affect how your liver breaks down other medicines (itraconazole, ketoconazole, voriconazole, and fluconazole)
- certain HIV medicines (atazanavir, indinavir)
- atorvastatin
- rosuvastatin
- etravirine
Hormonal birth control methods may interact with lamotrigine, an anti-seizure medicine used for epilepsy. This may increase the risk of seizures, so your healthcare provider may need to adjust the dose of lamotrigine.
Women on thyroid replacement therapy may need increased doses of thyroid hormone.
Know the medicines you take. Keep a list of them to show your doctor and pharmacist when you get a new medicine.
How should I use ethinyl estradiol and norelgestromin transdermal system?
- For detailed instructions, see the step-by-step instructions that come with ethinyl estradiol and norelgestromin transdermal system.
- Use ethinyl estradiol and norelgestromin transdermal system exactly as your healthcare provider tells you to use it.
- Wear 1 ethinyl estradiol and norelgestromin transdermal system patch at a time. Make sure you remove your old ethinyl estradiol and norelgestromin transdermal system patch before applying your new ethinyl estradiol and norelgestromin transdermal system patch.
- Do not skip using any ethinyl estradiol and norelgestromin transdermal system patches, even if you do not have sex often.
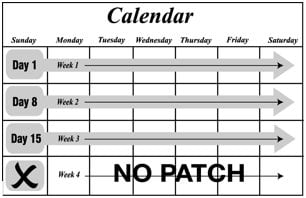
- Ethinyl estradiol and norelgestromin transdermal system is applied in a 4-week cycle.
- Apply your ethinyl estradiol and norelgestromin transdermal system patch 1 time each week for 3 weeks (21 total days).
- Apply each new ethinyl estradiol and norelgestromin transdermal system patch on the same day of the week. This day will be your "Patch Change Day." For example, if you apply your first ethinyl estradiol and norelgestromin transdermal system patch on a Monday, all of your ethinyl estradiol and norelgestromin transdermal system patches should be applied on a Monday.
- Do not apply your ethinyl estradiol and norelgestromin transdermal system patch during Week 4. Make sure you remove your old ethinyl estradiol and norelgestromin transdermal system patch. This is your patch-free week. Your menstrual period should start during your patch-free week.
- Begin a new 4 week cycle by applying a new ethinyl estradiol and norelgestromin transdermal system patch on the day after Week 4 ends. Repeat the cycle of 3 weekly applications followed by a patch-free week.
- Your ethinyl estradiol and norelgestromin transdermal system patch should never be off for more than 7 days in a row. If your ethinyl estradiol and norelgestromin transdermal system patch is off for more than 7 days in a row and you have sex during this time, you could become pregnant.
- If you miss a period you might be pregnant. Some women miss their periods or have light periods on hormonal birth control methods even when they are not pregnant. Call your healthcare provider if you miss one period and have not used your ethinyl estradiol and norelgestromin transdermal system patch every day or you miss two periods in a row.
What are the possible side effects of ethinyl estradiol and norelgestromin transdermal system?
Ethinyl estradiol and norelgestromin transdermal system may cause serious side effects, including:
- blood clots. Like pregnancy, hormonal birth control methods increase the risk of serious blood clots (see following graph), especially in women who have other risk factors, such as smoking, obesity, or age greater than 35. This increased risk is highest when you first start using hormonal birth control and when you restart the same or different hormonal birth control after not using it for a month or more. Some studies have reported that women who use norelgestromin and ethinyl estradiol transdermal system have a higher risk of getting a blood clot. Talk with your healthcare provider about your risk of getting a blood clot before using ethinyl estradiol and norelgestromin transdermal system or deciding which type of birth control is right for you.
It is possible to die or be permanently disabled from a problem caused by a blood clot, such as a heart attack or a stroke. Some examples of serious blood clots are blood clots in the:- legs (deep vein thrombosis)
- lungs (pulmonary embolus)
- eyes (loss of eyesight)
- heart (heart attack)
- brain (stroke)
To put the risk of developing a blood clot into perspective: If 10,000 women who are not pregnant and do not use hormonal birth control are followed for one year, between 1 and 5 of these women will develop a blood clot. The figure below shows the likelihood of developing a serious blood clot for women who are not pregnant and do not use hormonal birth control, for women who use hormonal birth control, for pregnant women, and for women in the first 12 weeks after delivering a baby.
Likelihood of Developing a Serious Blood Clot (Venous Thromboembolism [VTE])

Call your healthcare provider right away if you have:
- leg pain that will not go away
- sudden shortness of breath
- sudden blindness, partial or complete
- severe pain or pressure in your chest
- sudden, severe headache unlike your usual headaches
- weakness or numbness in an arm or leg, or trouble speaking
- yellowing of the skin or eyeballs
Other serious risks include
- liver problems including liver tumors
- gallbladder disease
- high blood pressure
The most common side effects of ethinyl estradiol and norelgestromin transdermal system are:
- breast symptoms (discomfort, swelling, or pain)
- nausea
- headache
- skin irritation, redness, pain, swelling, itching or rash at the patch application site
- stomach pain
- pain during menstruation
- vaginal bleeding and menstrual disorders, such as spotting or bleeding between periods
- mood, affect and anxiety disorders
Some women have spotting or light bleeding, breast tenderness, or feel sick to their stomach during norelgestromin and ethinyl estradiol transdermal system use. If these symptoms occur, do not stop using the ethinyl estradiol and norelgestromin transdermal system patch. The problem will usually go away. If it doesn't go away, check with your healthcare provider.
Less common side effects are:
- acne
- less sexual desire
- bloating or fluid retention
- blotchy darkening of your skin, especially your face
- high blood sugar, especially in women with diabetes
- high fat (cholesterol, triglycerides) levels in the blood
- depression, especially if you have had depression in the past. Call your healthcare provider immediately if you have any thoughts of harming yourself.
- problems tolerating contact lenses
- weight gain
Tell your healthcare provider about any side effect that bothers you or that does not go away.
These are not all the possible side effects of ethinyl estradiol and norelgestromin transdermal system. For more information, ask your healthcare provider or pharmacist.
Call your healthcare provider for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
General information about the safe and effective use of ethinyl estradiol and norelgestromin transdermal system
Medicines are sometimes prescribed for purposes other than those listed in Patient Information. Do not use ethinyl estradiol and norelgestromin transdermal system for a condition for which it was not prescribed. Do not give ethinyl estradiol and norelgestromin transdermal system to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about ethinyl estradiol and norelgestromin transdermal system that is written for health professionals.
For more information, contact Mylan Pharmaceuticals Inc. at 1-877-446-3679 (1-877-4-INFO-RX).
How should I store ethinyl estradiol and norelgestromin transdermal system?
- Store at room temperature between 20° to 25°C (68° to 77°F).
- Do not store ethinyl estradiol and norelgestromin transdermal system patches outside of their pouches. Apply immediately upon removal from the protective pouch.
- Do not store in the refrigerator or freezer.
- Used ethinyl estradiol and norelgestromin transdermal system patches still contain some active hormones. To throw away the ethinyl estradiol and norelgestromin transdermal system patch, fold the sticky side of the patch together, place it in a sturdy child-proof container, and place this container in the trash. Do not flush used ethinyl estradiol and norelgestromin transdermal system patches down the toilet.
- Return unused, unneeded, or expired patches to your pharmacist.
Keep ethinyl estradiol and norelgestromin transdermal system and all medicines out of the reach of children.
What are the ingredients in ethinyl estradiol and norelgestromin transdermal system?
Active ingredient: norelgestromin and ethinyl estradiol
Inactive ingredient: crospovidone, dipropylene glycol, fluoropolymer coated polyester film, light mineral oil, non-woven polyester fabric, oleyl alcohol, polyethylene/polyester film and polyisobutene adhesive. Each patch is printed with brown ink.