What is Lemtrada?
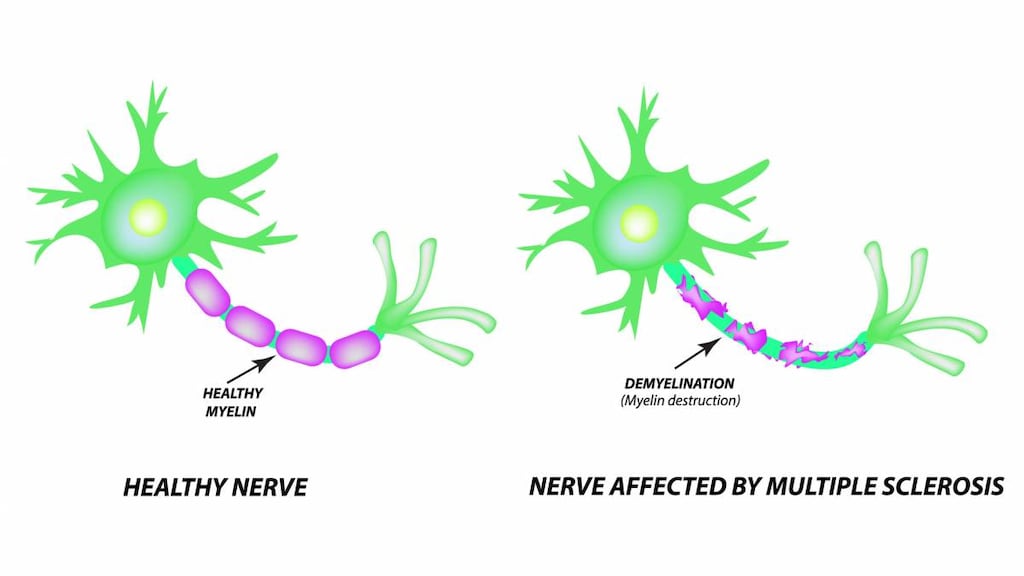
Lemtrada is a prescription medicine used to treat relapsing forms of multiple sclerosis (MS), to include relapsing-remitting disease and active secondary progressive disease, in adults.
Since treatment with Lemtrada can increase your risk of getting certain conditions and diseases, Lemtrada is generally prescribed for people who have tried 2 or more MS medicines that have not worked well enough. Lemtrada is not recommended for use in patients with clinically isolated syndrome (CIS).
It is not known if Lemtrada is safe and effective for use in children under 17 years of age.
What is the most important information I should know about Lemtrada?
Lemtrada can cause serious side effects, including:
1. Serious autoimmune problems. Some people receiving Lemtrada develop a condition where the immune cells in your body attack other cells or organs in the body (autoimmunity) which can be serious and may cause death. Serious autoimmune problems may include:
- immune thrombocytopenic purpura (ITP). Lemtrada may cause the number of platelets in your blood to be reduced (ITP). ITP can cause severe bleeding that may cause life-threatening problems. Call your healthcare provider right away if you have any of the following symptoms:
- easy bruising
- bleeding from a cut that is hard to stop
- coughing up blood
- heavier menstrual periods than normal
- bleeding from your gums or nose that is new or takes longer than usual to stop
- small, scattered spots on your skin that are red, pink, or purple
- kidney problems. Lemtrada may cause a serious kidney problem called anti-glomerular basement membrane disease. If this happens and you do not get treated, anti-glomerular basement membrane disease can lead to severe kidney damage, kidney failure that needs dialysis, a kidney transplant, or death. Call your healthcare provider right away if you have any of the following symptoms:
- swelling of your legs or feet
- blood in the urine (red or tea-colored urine)
- decrease in urine
- fatigue
- coughing up blood
Side effects may happen while you receive Lemtrada and for 4 years after you stop receiving Lemtrada. Your healthcare provider will order blood and urine tests before you receive, while you are receiving, and every month for 4 years after you receive your last Lemtrada infusion. You may need to continue these blood and urine tests after 4 years if you have any autoimmune signs or symptoms. The blood and urine tests will help your healthcare provider watch for signs and symptoms of serious autoimmune problems.
It is important to have your blood and urine tested, even if you are feeling well and do not have any symptoms from Lemtrada and your multiple sclerosis. This may help your healthcare provider find any problems early.
2. Serious infusion reactions. Lemtrada can cause serious infusion reactions that may cause death. Serious infusion reactions may happen while you receive, or up to 24 hours or longer after you receive Lemtrada.
You will receive your infusion at a healthcare facility with equipment and staff trained to manage infusion reactions. You will be watched while you receive and for at least 2 hours after you receive Lemtrada. It is important that you stay at the infusion center for at least 2 hours after your infusion is finished or longer if your healthcare provider decides you need to stay longer. If a serious infusion reaction happens while you are receiving Lemtrada, your infusion may be stopped.
Tell your healthcare provider right away if you have any of the following symptoms of a serious infusion reaction during the infusion, and after you have left the healthcare facility:
- swelling in your mouth or throat
- trouble breathing
- weakness
- fast, slow, or irregular heartbeat
- chest pain
- rash
To lower your chances of getting a serious infusion reaction, your healthcare provider will give you a medicine called corticosteroids before your first 3 infusions of a treatment course. You may also be given other medicines before or after the infusion to try to reduce your chances of these reactions or to treat them after they happen.
3. Stroke and tears in your arteries that supply blood to your brain (carotid and vertebral arteries). Some people have had serious and sometimes deadly strokes and tears in their carotid or vertebral arteries within 3 days of receiving Lemtrada. Get help right away if you have any of the following symptoms that may be signs of a stroke or tears in your carotid or vertebral arteries:
- drooping of parts of your face
- sudden severe headache
- neck pain
- weakness on one side
- difficulty with speech
4. Certain cancers. Receiving Lemtrada may increase your chance of getting some kinds of cancers, including thyroid cancer, skin cancer (melanoma), and blood cancers called lymphoproliferative disorders and lymphoma. Call your healthcare provider if you have the following symptoms that may be a sign of thyroid cancer:
- new lump
- swelling in your neck
- pain in the front of your neck
- hoarseness or other voice changes that do not go away
- trouble swallowing or breathing
- cough that is not caused by a cold
You should have your skin checked before you start receiving Lemtrada and each year while you are receiving treatment to monitor symptoms of skin cancer.
Because of your risk of autoimmunity, infusion reactions, and the risk of some kinds of cancers, Lemtrada is only available through a restricted program called the Lemtrada Risk Evaluation and Mitigation Strategy (REMS) Program. Call 1-855-676-6326 to enroll in the Lemtrada REMS Program.
- You and your healthcare provider must be enrolled in the Lemtrada REMS Program.
- Lemtrada can only be given at a certified healthcare facility that participates in the Lemtrada REMS Program. Your healthcare provider can give you information on how to find a certified healthcare facility.
- Read the Lemtrada REMS "Lemtrada Treatment and Infusion Reactions Patient Guide" after you are enrolled in the program.
- Carry your Lemtrada REMS Patient Safety Information Card with you in case of an emergency.
Who should not use Lemtrada?
Do not receive Lemtrada if you:
- are allergic to alemtuzumab or to any of the inactive ingredients in Lemtrada. See below for a complete list of ingredients in Lemtrada.
- are infected with human immunodeficiency virus (HIV)
- have an active infection
What should I tell my healthcare provider before using Lemtrada?
Before receiving Lemtrada, tell your healthcare provider if you:
- have bleeding problems.
- have thyroid problems.
- have kidney problems.
- have a recent history of infection.
- are taking a medicine called Campath. Alemtuzumab, the active ingredient in Lemtrada, is the same drug as Campath.
- have received a live vaccine in the past 6 weeks before receiving Lemtrada or plan to receive any live vaccines. Ask your healthcare provider if you are not sure if your vaccine is a live vaccine.
- are pregnant or plan to become pregnant. Lemtrada may harm your unborn baby.
- There is a pregnancy surveillance program for people who are exposed to Lemtrada during pregnancy. The purpose of the program is to collect information about the health of pregnant people exposed to Lemtrada and their babies. If you become pregnant, inform your healthcare provider.
- you should use birth control while receiving Lemtrada and for 4 months after your course of treatment.
- are breastfeeding or plan to breastfeed. It is not known if Lemtrada passes into your breast milk. You and your healthcare provider should decide if you should receive Lemtrada or breastfeed.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
Lemtrada and other medicines may affect each other causing side effects. Especially tell your healthcare provider if you take medicines that increase your chance of getting infections, including medicines used to treat cancer or to control your immune system.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist when you get a new medicine.
How should I use Lemtrada?
- Lemtrada is given through a needle placed in your vein (IV infusion).
- It takes about 4 hours to receive a full dose of Lemtrada each day.
- You will receive Lemtrada over 2 or more treatment courses.
- You will receive Lemtrada for 5 days in a row (consecutive) for the first treatment course and then for 3 days in a row (consecutive) about 1 year later for your second treatment course.
- Additional Lemtrada treatment courses, if needed, may be given for 3 days in a row (consecutive) at least 1 year after the prior treatment course.
What are the possible side effects of Lemtrada?
Lemtrada may cause serious side effects including:
- See "What is the most important information I should know about Lemtrada?"
- thyroid problems. Some people who receive Lemtrada may get thyroid problems including an overactive thyroid (hyperthyroidism) or an underactive thyroid (hypothyroidism). Your healthcare provider will do blood tests to check how your thyroid is working. Call your healthcare provider if you have any of the symptoms of thyroid problems.
- Symptoms of hyperthyroidism may include:
- excessive sweating
- unexplained weight loss
- fast heartbeat
- eye swelling
- nervousness
- Symptoms of hypothyroidism may include:
- unexplained weight gain
- feeling cold
- worsening tiredness
- constipation
- Symptoms of hyperthyroidism may include:
- low blood counts (cytopenias). Lemtrada may cause a decrease in some types of blood cells. Some people with these low blood counts have increased infections. Symptoms of cytopenias may include:
- weakness
- chest pain
- yellowing of the skin or whites of eyes (jaundice)
- dark urine
- fast heartbeat
Your healthcare provider will do blood tests to check for cytopenias. Call your healthcare provider right away if you have symptoms listed above.
- inflammation of the liver. Call your healthcare provider right away if you have symptoms such as unexplained nausea, stomach pain, tiredness, loss of appetite, yellowing of skin or whites of eyes, or bleeding or bruising more easily than normal.
- hemophagocytic lymphohistiocytosis (HLH). Lemtrada may increase the risk of a type of overactivity of the immune system (hemophagocytic lymphohistiocytosis) that can be fatal, especially if not diagnosed and treated early. Call your healthcare provider right away if you have symptoms such as fever, swollen glands, skin rash, or new nervous system problems, such as seizures, changes in your thinking or level of alertness, or new or worsening unsteadiness or trouble walking. These symptoms have happened in people taking Lemtrada about 13 months to 33 months after they started taking Lemtrada.
- adult onset still's disease (AOSD). Adult onset still's disease (AOSD) is a rare condition that can cause a high fever lasting more than 1 week, pain, stiffness with or without swelling in multiple joints, and/or a skin rash. If you experience a combination of these symptoms, contact your healthcare provider immediately.
- thrombotic thrombocytopenic purpura (TTP). Thrombotic thrombocytopenic purpura (TTP) can occur with Lemtrada. TTP is a blood clotting problem where blood clots can form in blood vessels anywhere in the body. TTP needs to be treated in a hospital right away, because it can cause death. Get medical help right away if you have any of these symptoms:
- purplish spots (called purpura) on the skin or in the mouth (mucous membranes) due to bleeding under the skin
- your skin or the whites of your eyes are yellow (jaundice)
- you feel tired or weak
- your skin looks very pale
- fever
- fast heart rate or feeling short of breath
- headache
- speech changes
- confusion
- vision changes
- seizure
- low amount of urine or dark urine, or urine that has blood in it
- stomach area (abdominal) pain
- nausea, vomiting, or diarrhea
- autoimmune encephalitis (AIE). Autoimmune encephalitis (AIE), a brain disorder, can occur after receiving Lemtrada and may include symptoms that may seem like an MS relapse. Call your healthcare provider right away if you have any of the following symptoms:
- personality changes
- mood changes
- seeing things that are not there (hallucinations)
- agitation
- short term memory loss
- confusion
- movement disorders
- seizure
- bleeding disorder (acquired hemophilia A). Lemtrada may cause a bleeding disorder called acquired hemophilia A. Call your healthcare provider right away if you have any of the following symptoms:
- bruising
- nose bleeds
- painful or swollen joints
- bleeding from a cut that may take longer than usual to stop
- blood in urine
- dark or bloody stools
- serious infections. Lemtrada may cause you to have serious infections while you receive and after receiving a treatment course. Serious infections may include:
- listeria. People who receive Lemtrada have an increased chance of getting an infection caused by the bacteria, listeria, which can lead to significant complications or death. Avoid foods that may be a source for listeria (for example, deli meat, unpasteurized milk and cheese products, soft cheeses, or undercooked meat, seafood or poultry) or make sure that the food you eat which may contain listeria is heated well if you receive treatment with Lemtrada.
- herpes viral infections. Some people taking Lemtrada have an increased chance of getting herpes viral infections. Your healthcare provider will prescribe medicines to reduce your chances of getting these infections. Take these medicines exactly as your healthcare provider tells you to.
- human papilloma virus (HPV). Females have an increased chance of getting a cervical HPV infection. If you are a female, you should have an HPV screening each year.
- tuberculosis. Your healthcare provider should check you for tuberculosis before you receive Lemtrada.
- fungal infections.
Call your healthcare provider right away if you have symptoms of a serious infection, such as fever or swollen glands. You may need to go to the hospital for treatment if you get a serious infection. It is important to tell the healthcare providers that you have received Lemtrada.
Talk to your healthcare provider before you get vaccinations after receiving Lemtrada. Certain vaccinations may increase your chances of getting infections.
- Progressive multifocal leukoencephalopathy (PML). A rare brain infection that usually leads to death or severe disability has been reported with Lemtrada. Symptoms of PML get worse over days to weeks. It is important that you call your doctor right away if you have any new or worsening medical problems that have lasted several days, including problems with:
- thinking
- eyesight
- strength
- balance
- weakness on 1 side of your body
- using your arms or legs
- Inflammation of the gallbladder without gallstones (acalculous cholecystitis). Lemtrada may increase your chance of getting inflammation of the gallbladder without gallstones, a serious medical condition that can be life-threatening. Call your healthcare provider right away if you have any of the following symptoms of acalculous cholecystitis, which may include:
- stomach pain or discomfort
- fever
- nausea or vomiting
- swelling of lung tissue (pneumonitis). Some people have had swelling of the lung tissue while receiving Lemtrada. Call your healthcare provider right away if you have the following symptoms:
- shortness of breath
- cough
- wheezing
- chest pain or tightness
- coughing up blood
The most common side effects of Lemtrada include:
- rash
- headache
- thyroid problems
- fever
- swelling of your nose and throat (nasopharyngitis)
- nausea
- urinary tract infection
- feeling tired
- trouble sleeping
- upper respiratory tract infection
- herpes viral infection
- hives
- itching
- fungal infection
- joint pain
- pain in your arms or legs
- back pain
- diarrhea
- sinus infection
- mouth pain or sore throat
- tingling sensation
- dizziness
- stomach pain
- sudden redness in face, neck, or chest
- vomiting
Tell your healthcare provider if you have any side effect that bothers you or that does not go away.
These are not all the possible side effects of Lemtrada. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to the FDA at 1-800-FDA-1088.
General information about the safe and effective use of Lemtrada
This guide summarizes the most important information about Lemtrada. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about Lemtrada that is written for health professionals.
For more information, go to www.LemtradaREMS.com or call Genzyme at 1-855-676-6326.
What are the ingredients in Lemtrada?
Active ingredient: alemtuzumab
Inactive ingredients: dibasic sodium phosphate, disodium edetate dihydrate, polysorbate 80, potassium chloride, potassium dihydrogen phosphate, sodium chloride, and Water for Injection, USP.