What is Ocrevus?
Ocrevus is a prescription medicine used to treat:
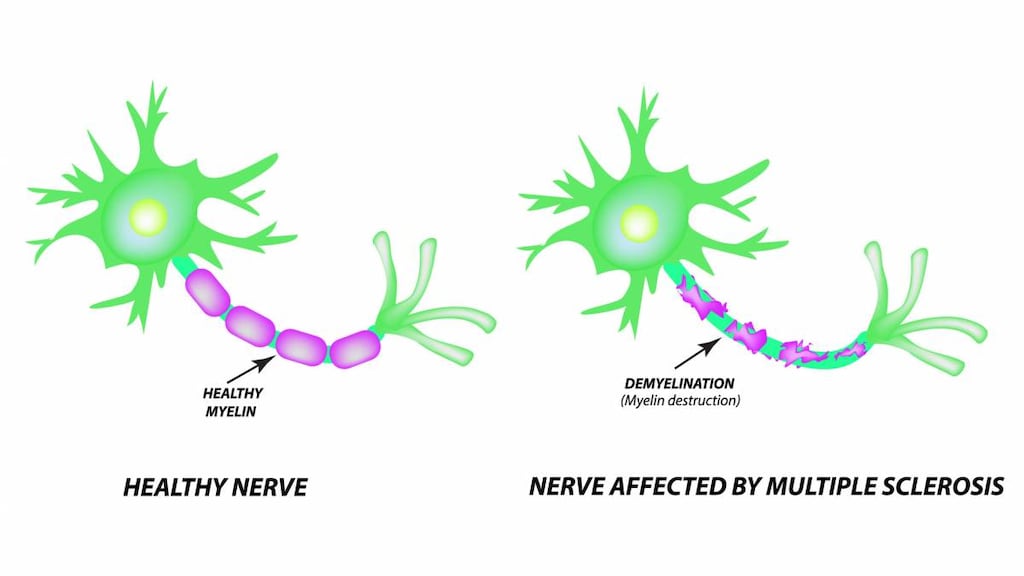
- Relapsing forms of multiple sclerosis (MS), to include clinically isolated syndrome, relapsing-remitting disease, and active secondary progressive disease, in adults
- Primary progressive MS, in adults.
It is not known if ocrevus is safe or effective in children.
What is the most important information I should know about Ocrevus?
Ocrevus can cause serious side effects, including:
- Infusion reactions: Ocrevus can cause infusion reactions that can be serious and require you to be hospitalized. You will be monitored during your infusion and for at least 1 hour after each infusion of Ocrevus for signs and symptoms of an infusion reaction. Tell your healthcare provider or nurse if you get any of these symptoms:
- itchy skin
- rash
- hives
- tiredness
- coughing or wheezing
- trouble breathing
- throat irritation or pain
- feeling faint
- fever
- redness on your face (flushing)
- nausea
- headache
- swelling of the throat
- dizziness
- shortness of breath
- fatigue
- fast heart beat
These infusion reactions can happen for up to 24 hours after your infusion. It is important that you call your healthcare provider right away if you get any of the signs or symptoms listed above after each infusion.
If you get infusion reactions, your healthcare provider may need to stop or slow down the rate of your infusion.
- Infection
See ”What are the possible side effects of Ocrevus?" for more information about side effects.
- Ocrevus increases your risk of getting upper respiratory tract infections, lower respiratory tract infections, skin infections, and herpes infections. Infections are a common side effect, which can be serious. Tell your healthcare provider if you have an infection or have any of the following signs of infection including fever, chills, or a cough that does not go away. Signs of herpes infection include:
- cold sores
- shingles
- genital sores
- skin rash
- pain
- itching
Signs of a more serious herpes infection include:- changes in vision
- eye redness or eye pain
- severe or persistent headache
- stiff neck
- confusion
- Ocrevus increases your risk of getting upper respiratory tract infections, lower respiratory tract infections, skin infections, and herpes infections. Infections are a common side effect, which can be serious. Tell your healthcare provider if you have an infection or have any of the following signs of infection including fever, chills, or a cough that does not go away. Signs of herpes infection include:
Signs of infection can happen during treatment or after you have received your last dose of Ocrevus. Tell your healthcare provider right away if you have an infection. Your healthcare provider should delay your treatment with Ocrevus until your infection is gone.
- Progressive Multifocal Leukoencephalopathy (PML): Although no cases have been seen with Ocrevus treatment in clinical trials, PML may happen with Ocrevus. PML is a rare brain infection that usually leads to death or severe disability. Tell your healthcare provider right away if you have any new or worsening neurologic signs or symptoms. These may include problems with thinking, balance, eyesight, weakness on 1 side of your body, strength, or using your arms or legs.
- Hepatitis B virus (HBV) reactivation: Before starting treatment with Ocrevus, your healthcare provider will do blood tests to check for hepatitis B viral infection. If you have ever had hepatitis B virus infection, the hepatitis B virus may become active again during or after treatment with Ocrevus. Hepatitis B virus becoming active again (called reactivation) may cause serious liver problems including liver failure or death. Your healthcare provider will monitor you if you are at risk for hepatitis B virus reactivation during treatment and after you stop receiving Ocrevus.
- Weakened immune system: Ocrevus taken before or after other medicines that weaken the immune system could increase your risk of getting infections.
- Decreased immunoglobulins: Ocrevus may cause a decrease in some types of immunoglobulins. Your healthcare provider will do blood tests to check your blood immunoglobulin levels.
See "What are the possible side effect of Ocrevus?" for more information about side effects.
Who should not use Ocrevus?
- Do not receive Ocrevus if you have an active hepatitis B virus (HBV) infection.
- Do not receive Ocrevus if you have had a life threatening allergic reaction to Ocrevus. Tell your healthcare provider if you have had an allergic reaction to Ocrevus or any of its ingredients in the past. See below for a complete list of ingredients in Ocrevus.
What should I tell my healthcare provider before using Ocrevus?
Before receiving Ocrevus, tell your healthcare provider about all of your medical conditions, including if you:
- have or think you have an infection. See "What is the most important information I should know about Ocrevus?"
- have ever taken, take, or plan to take medicines that affect your immune system, or other treatments for MS. These medicines could increase your risk of getting an infection.
- have ever had hepatitis B or are a carrier of the hepatitis B virus.
- have had a recent vaccination or are scheduled to receive any vaccinations.
- You should receive any required 'live' or 'live-attenuated' vaccines at least 4 weeks before you start treatment with Ocrevus. You should not receive 'live' or 'live-attenuated' vaccines while you are being treated with Ocrevus and until your healthcare provider tells you that your immune system is no longer weakened.
- When possible, you should receive any 'non-live' vaccines at least 2 weeks before you start treatment with Ocrevus. If you would like to receive any non-live (inactivated) vaccines, including the seasonal flu vaccine, while you are being treated with Ocrevus, talk to your healthcare provider.
- If you have a baby and you received Ocrevus during your pregnancy, it is important to tell your baby's healthcare provider about receiving Ocrevus so they can decide when your baby should be vaccinated.
- are pregnant, think that you might be pregnant, or plan to become pregnant. It is not known if Ocrevus will harm your unborn baby. You should use birth control (contraception) during treatment with Ocrevus and for 6 months after your last infusion of Ocrevus. Talk with your healthcare provider about what birth control method is right for you during this time.
- Pregnancy Registry. There is a pregnancy registry for women who take Ocrevus during pregnancy. If you become pregnant while receiving Ocrevus, tell your healthcare provider right away. Talk to your healthcare provider about registering with the Ocrevus Pregnancy Registry. The purpose of this registry is to collect information about your health and your baby's health. Your healthcare provider can enroll you in this registry by calling 1-833-872-4370 or visiting www.ocrevuspregnancyregistry.com.
- are breastfeeding or plan to breastfeed. It is not known if Ocrevus passes into your breast milk. Talk to your healthcare provider about the best way to feed your baby if you take Ocrevus.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements.
How should I use Ocrevus?
- Ocrevus is given through a needle placed in your vein (intravenous infusion) in your arm.
- Before treatment with Ocrevus, your healthcare provider will give you a corticosteroid medicine and an antihistamine to help reduce infusion reactions (make them less frequent and less severe). You may also receive other medicines to help reduce infusion reactions. See "What is the most important information I should know about Ocrevus?"
- Your first full dose of Ocrevus will be given as 2 separate infusions, 2 weeks apart. Each infusion will last about 2 hours and 30 minutes.
- Your next doses of Ocrevus will be given as 1 infusion every 6 months. These infusions will last about 2 hours to 3 hours and 30 minutes depending on the infusion rate prescribed by your healthcare provider.
What are the possible side effects of Ocrevus?
Ocrevus may cause serious side effects, including:
- See "What is the most important information I should know about Ocrevus?"
- Risk of cancers (malignancies) including breast cancer. Follow your healthcare provider's instructions about standard screening guidelines for breast cancer.
These are not all the possible side effects of Ocrevus.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
General information about the safe and effective use of Ocrevus
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use Ocrevus for a condition for which it was not prescribed. Do not give Ocrevus to other people, even if they have the same symptoms that you have. It may harm them. You can ask your pharmacist or healthcare provider for information about Ocrevus that is written for health professionals.
What are the ingredients in Ocrevus?
Active ingredient: ocrelizumab
Inactive ingredients: glacial acetic acid, polysorbate 20, sodium acetate trihydrate, trehalose dihydrate.
For more information, go to www.OCREVUS.com or call 1-844-627-3887.