What is Qsymia?
- Qsymia is a prescription medicine that contains phentermine and topiramate extended-release that may help some obese adults or some overweight adults who also have weight-related medical problems lose weight and keep the weight off.
- Qsymia should be used with a reduced calorie diet and increased physical activity.
- It is not known if Qsymia changes your risk of heart problems or stroke or of death due to heart problems or stroke.
- It is not known if Qsymia is safe and effective when taken with other prescription and over-the-counter medicines, or herbal weight loss products.
- It is not known if Qsymia is safe and effective in children under 18 years old.
- Qsymia is a federally controlled substance (CIV) because it contains phentermine and can be abused or lead to drug dependence. Keep Qsymia in a safe place, to protect it from theft. Never give your Qsymia to anyone else, because it may cause death or harm them. Selling or giving away Qsymia is against the law.
What is the most important information I should know about Qsymia?
Qsymia can cause serious side effects, including:
- Birth defects (cleft lip and cleft palate). If you take Qsymia during pregnancy, your baby has a higher risk for birth defects called cleft lip and cleft palate. These defects can begin early in pregnancy, even before you know you are pregnant.
Patients who are pregnant must not take Qsymia.
Patients who can become pregnant should:- Have a pregnancy test before taking Qsymia and every month while taking Qsymia.
- Use effective birth control (contraception) consistently while taking Qsymia. Talk to your healthcare provider about how to prevent pregnancy.
- FDA MedWatch at 1-800-FDA-1088, and
Because of the risk for birth defects (cleft lip and cleft palate), Qsymia is available through a restricted program called the Qsymia Risk Evaluation and Mitigation Strategy (REMS). Qsymia is only available through certified pharmacies that participate in the Qsymia REMS program. Your healthcare provider can give you information about how to find a certified pharmacy. For more information, go to www.QsymiaREMS.com or call 1-888-998-4887
- Increases in heart rate. Qsymia can increase your heart rate at rest. Your healthcare provider should check your heart rate while you take Qsymia. Tell your healthcare provider if you experience, while at rest, a racing or pounding feeling in your chest lasting several minutes when taking Qsymia.
- Suicidal thoughts or actions. Topiramate, an ingredient in Qsymia, may cause you to have suicidal thoughts or actions. Call your healthcare provider right away if you have any of these symptoms, especially if they are new, worse, or worry you:
- thoughts about suicide or dying
- attempts to commit suicide
- new or worse depression
- new or worse anxiety
- feeling agitated or restless
- panic attacks
- trouble sleeping (insomnia)
- new or worse irritability
- acting aggressive, being angry, or violent
- acting on dangerous impulses
- an extreme increase in activity and talking (mania)
- other unusual changes in behavior or mood
- Serious eye problems which include:
- any sudden decrease in vision, with or without eye pain and redness,
- a blockage of fluid in the eye causing increased pressure in the eye (secondary angle closure glaucoma).
Qsymia can have other serious side effects. See " What are the possible side effects of Qsymia?"
Who should not take Qsymia?
Do not take Qsymia if you:
- are pregnant, planning to become pregnant, or become pregnant during Qsymia treatment.
- have glaucoma.
- have thyroid problems (hyperthyroidism).
- are taking certain medicines called monoamine oxidase inhibitors (MAOIs) or have taken MAOIs in the past 14 days.
- are allergic to topiramate, sympathomimetic amines such as phentermine, or any of the ingredients in Qsymia. See below for a complete list of ingredients in Qsymia.
What should I tell my healthcare provider before taking Qsymia?
Before taking Qsymia, tell your healthcare provider about all of your medical conditions, including if you:
- have had a heart attack or stroke.
- have or have had an abnormal heart rhythm.
- have or have had depression, mood problems, or suicidal thoughts or behavior.
- have eye problems, especially glaucoma. See “Who should not take Qsymia?”
- have a history of too much acid in the blood (metabolic acidosis) or a condition that puts you at higher risk for metabolic acidosis such as:
- chronic diarrhea, surgery, a diet high in fat and low in carbohydrates (ketogenic diet), weak, brittle, or soft bones (osteomalacia, osteoporosis, osteopenia), or decreased bone density
- have type 2 diabetes and take medicine to control your blood sugar.
- have kidney problems, kidney stones, or are getting kidney dialysis.
- have liver problems.
- have seizures or convulsions (epilepsy).
- are breastfeeding or plan to breastfeed. Qsymia can pass into your breast milk and may harm your baby. You and your healthcare provider should decide if you will take Qsymia or breastfeed. You should not do both.
Tell your healthcare provider about all the medicines you take, including prescription and over-the-counter medicines, vitamins, and herbal supplements. Qsymia taken with other medicines may affect how each medicine works and may cause side effects.
Especially tell your healthcare provider if you take:
- Birth control pills. Tell your healthcare provider if your menstrual bleeding changes while you are taking birth control pills that contain both estrogen and progestin (combination oral contraceptives) and Qsymia.
- Water pills (diuretics) such as hydrochlorothiazide (HCTZ).
- Any medicines that impair or decrease your thinking, concentration, or muscle coordination.
- Carbonic anhydrase inhibitors such as Zonegran (zonisamide), Diamox (acetazolamide) or Neptazane (methazolamide).
- Seizure medicines such as valproic acid (Depakene or Depakote).
Ask your healthcare provider or pharmacist for a list of these medicines, if you are not sure.
Know the medicines you take. Keep a list of them to show your healthcare provider and pharmacist each time you get a new medicine. Do not start a new medicine without talking to your healthcare provider.
How should I take Qsymia?
- Your healthcare provider should start you on a diet and exercise program when you start taking Qsymia. Stay on this program while you are taking Qsymia.
- Do not change your dose without talking to your healthcare provider.
- Qsymia can be taken with or without food.
- If you miss a dose of Qsymia, wait until the next morning to take your usual dose of Qsymia. Do not double your dose.
- To start treatment with Qsymia
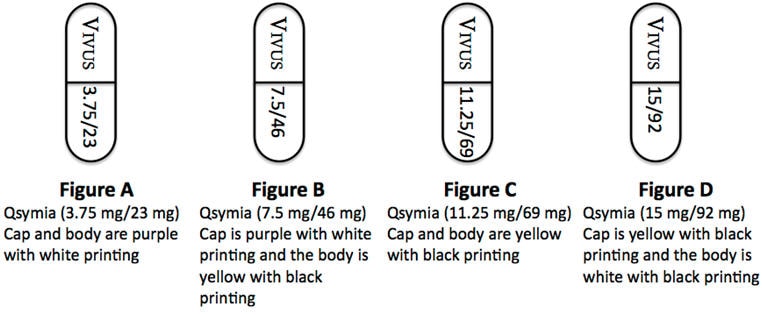
- Take 1 Qsymia 3.75 mg/23 mg capsule (Figure A) 1 time each morning for the first 14 days.
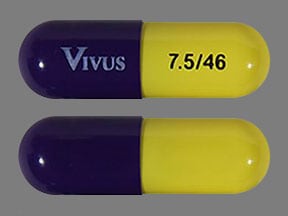
- After taking Qsymia 3.75 mg/23 mg capsule for 14 days, then take 1 Qsymia 7.5 mg/46 mg capsule (Figure B) 1 time each morning.
- After taking Qsymia for 12 weeks
- Your healthcare provider should either tell you to stop taking Qsymia or increase your dose of Qsymia if you do not lose a certain amount of weight within the first 12 weeks of treatment at the recommended dose.
- If your healthcare provider increases the dose of Qsymia
- Take 1 Qsymia 11.25 mg/69 mg capsule (Figure C) 1 time each morning for 14 days.
- After taking 14 days of Qsymia 11.25 mg/69 mg capsule, then take 1 Qsymia 15 mg/92 mg capsule (Figure D) 1 time each morning.
- Stopping Qsymia treatment
Your healthcare provider should tell you to stop taking Qsymia if you have not lost a certain amount of weight after an additional 12 weeks of treatment on the higher dose.
Do not stop taking Qsymia without talking to your healthcare provider. Stopping Qsymia suddenly can cause serious problems, such as seizures. Your healthcare provider will tell you how to stop taking Qsymia slowly.
If you take too much Qsymia, call your healthcare provider or go to the nearest emergency room right away.
What should I avoid while taking Qsymia?
- Do not get pregnant while taking Qsymia. See “What is the most important information I should know about Qsymia.”
- Do not drink alcohol while taking Qsymia. Qsymia and alcohol can affect each other causing side effects such as sleepiness or dizziness.
- Do not drive a car, operate heavy machinery, or do other dangerous activities until you know how Qsymia affects you. Qsymia can slow your thinking and motor skills, and may affect vision.
What are the possible side effects of Qsymia?
- See “What is the most important information I should know about Qsymia?" above.
- Mood changes and trouble sleeping. Qsymia may cause depression or mood problems, and trouble sleeping. Tell your healthcare provider if symptoms occur.
- Concentration, memory, and speech difficulties. Qsymia may affect how you think and cause confusion, problems with concentration, attention, memory, or speech. Tell your healthcare provider if symptoms occur.
- Increases of acid in bloodstream (metabolic acidosis). If left untreated, metabolic acidosis can cause brittle or soft bones (osteoporosis, osteomalacia, osteopenia), kidney stones, can slow the rate of growth in children, and may possibly harm your baby if you are pregnant. Metabolic acidosis can happen with or without symptoms. Sometimes people with metabolic acidosis will:
- feel tired
- not feel hungry (loss of appetite)
- feel changes in heartbeat
- have trouble thinking clearly
- Low blood sugar (hypoglycemia) in people with type 2 diabetes mellitus who also take medicines used to treat type 2 diabetes mellitus. Weight loss can cause low blood sugar in people with type 2 diabetes mellitus who also take medicines used to treat type 2 diabetes mellitus (such as insulin or sulfonylureas). You should check your blood sugar before you start taking Qsymia and while you take Qsymia.
- Possible seizures if you stop taking Qsymia too fast. Seizures may happen in people who may or may not have had seizures in the past if you stop Qsymia too fast. Your healthcare provider will tell you how to stop taking Qsymia slowly.
- Kidney stones. Drink plenty of fluids when taking Qsymia to help decrease your chances of getting kidney stones. If you get severe side or back pain, or blood in your urine, call your healthcare provider
- Decreased sweating and increased body temperature (fever). People should be watched for signs of decreased sweating and fever, especially in hot temperatures. Some people may need to be hospitalized for this condition.
Common side effects of Qsymia include:
- numbness or tingling in the hands, arms, feet, or face (paraesthesia)
- dizziness
- change in the way foods taste or loss of taste (dysgeusia)
- trouble sleeping (insomnia)
- constipation
- dry mouth
Tell your healthcare provider if you have any side effect that bothers you or does not go away.
These are not all of the possible side effects of Qsymia. For more information, ask your healthcare provider or pharmacist.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
You can also report side effects to VIVUS at 1-888 998-4887.
Qsymia Images
General information about the safe and effective use of Qsymia
Medicines are sometimes prescribed for purposes other than those listed in a Medication Guide. Do not use Qsymia for a condition for which it was not prescribed. Do not give Qsymia to other people, even if they have the same symptoms you have. It may harm them.
This guide summarizes the most important information about Qsymia. If you would like more information, talk with your healthcare provider. You can ask your pharmacist or healthcare provider for information about Qsymia that is written for health professionals.
For more information, go to www.QsymiaREMS.com or call 1-888-998-4887.
How should I store Qsymia?
- Store Qsymia at room temperature between 59°F to 77°F (15°C to 25°C).
Keep Qsymia and all medicines out of the reach of children.
What are the ingredients in Qsymia?
Active Ingredient: phentermine hydrochloride and topiramate
Inactive Ingredients: methylcellulose, sucrose, starch, microcrystalline cellulose, ethylcellulose, povidone, gelatin, talc, titanium dioxide, FD&C Blue #1, FD&C Red #3, FD&C Yellow #5 and #6, and pharmaceutical black and white inks.