Cystic Acne 101: Causes and Treatments
Nearly everyone has had at least a pimple or two on their face — and most likely at the most inopportune time. In fact, most people suffer from breakouts or acne in their teens and young adult years, according to the National Institute of Arthritis and Musculoskeletal and Skin Diseases, and about 80 percent of people between the ages of 11 and 30 have breakouts at some point.
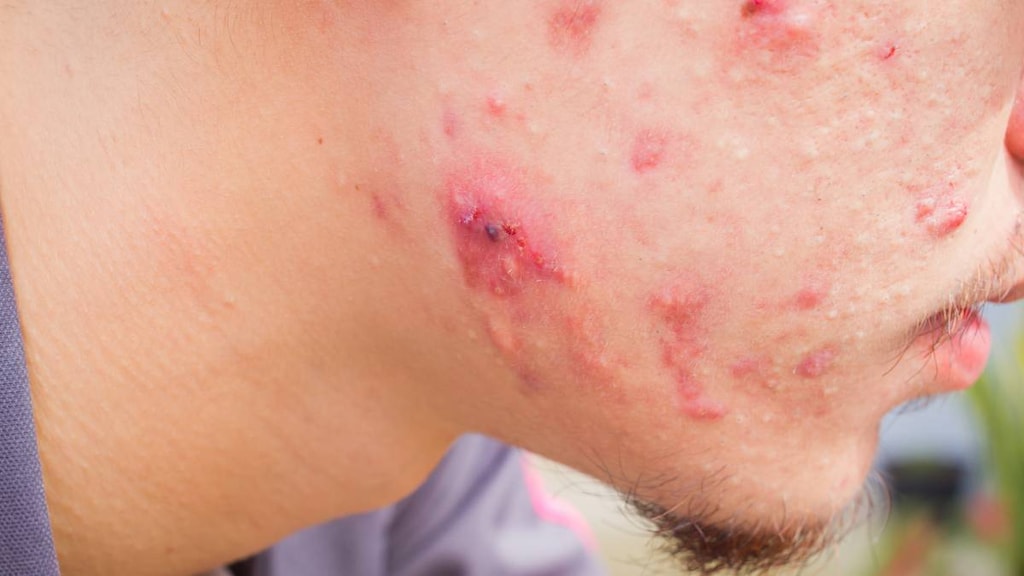
There are lots of different types of pimples, too: blackheads, whiteheads, papules (small pink, tender bumps) and nodules for example. Then there are cysts or cystic acne, which is one of the most severe types.
Cysts can form when your pores get blocked and super irritated. A whitish-yellowish liquid known as pus fills the cysts and makes them appear infected and inflamed. Cystic acne can be very painful and leave scars. The cysts can be as small as a pencil eraser. Or even larger than one.
What causes cystic acne
You're most likely to get acne on your face. That’s true of cystic acne as well. But you also can develop cystic acne on your chest, back and even your buttocks. This is where you have the most sebaceous glands. Sebaceous glands produce sebum, an oily substance. Canals known as follicles connect your pores to these glands. Sometimes, the oil that’s produced moves any dead skin cells along these canals to the surface of your skin. Follicles also contain thin hairs. The oil, dead skin and hair can cluster together and plug up or block your pores. Bacteria can get in this plug and cause swelling. As the plug breaks down, you can break out.
You can have cystic acne but also blackheads and whiteheads at the same time, too. And once you’re able to get your cystic acne to clear, you may be left with scars.
The most common trigger for all types of acne, including cystic, is puberty. That’s when hormones rage. During puberty, boys and girls produce more hormones known as androgens. These hormones cause your sebaceous glands to enlarge and to subsequently increase their production of sebum. More sebum, worse acne, according to the Mayo Clinic. Pregnancy also affects hormone production and can worsen acne.
Other factors that may make your acne worse include:
- Your diet. Diets that emphasize carbohydrates — bread, bagels, potato chips — may increase acne, according to the Mayo Clinic. However, greasy foods appear to have little, if any, effect on who has acne and how severe it is.
- Your stress levels. Being stressed won’t cause you to break out. However, if your face is already covered in pimples and cysts, stress can make them worse.
How to get rid of cystic acne
Because cystic acne is unsightly and occurs at a vulnerable time in your life, it can cause you to become anxious and depressed. You may not wish to hang out with your friends or participate in school activities.
But you don’t have to hide if you have cystic acne. A dermatologist can help you treat it and, while your treatment is likely to take some time to work, it will. Treatment should help you feel and look better and help prevent your cysts from leaving scars.
Those over-the-counter medicines you can buy at the local drugstore aren’t likely to be effective for your severe acne. You likely need a dermatologist to treat your cystic acne.
Here are treatment options that your dermatologist may suggest:
Topical Medications
- Retinoids and retinoid-like drugs. These work by stopping the development of new breakouts and encouraging new cells to form. They also unplug pimples. Options include tretinoin, adapalene and tazarotene.
- Antibiotics. Antibiotics are used to help control bacteria and to lower inflammation. Antibiotics can be applied topically. The goal of antibiotics you apply to your skin is to reduce bacteria and unclog pores. You may need to experiment with different antibiotics until you find one that works well for you and one that works long-term.
- Salicylic acid and azelaic acid. Salicylic acid may help prevent hair follicles from plugging pores. You can get it as a wash-off or leave-on product. A 20 percent azelaic acid cream seems to reduce acne when used twice a day for at least four weeks. It may work even better when used in combination with the antibiotic erythromycin. However, you may find it discolors your skin and can be irritating.
- Dapsone. This is a gel that should be applied twice a day and can help inflammatory acne, especially in adult women. It may cause redness and dryness.
Oral Medications
- Antibiotics. Oral antibiotics help reduce the redness and lessen swelling. You may be prescribed an oral as well as a topical antibiotic.
- Isotretinoin. If antibiotics, your first line of attack, don’t help, your dermatologist might recommend isotretinoin, a pretty potent medicine. Isotretinoin attacks all the causes of severe acne at the same time: bacteria, clogged pores, excess oil and inflammation. The vast majority — 85 percent — of patients respond well to isotretinoin, according to the American Academy of Dermatology (AAD). Not only does their skin clear, but their acne doesn’t return, and that’s usually after only one course of treatment.
The drawback: Isotretinoin has a long list of possible side effects, and you will have to decide whether you’re willing to risk them. Because of the possible side effects, you are required to be monitored while taking it. Isotretinoin also can cause birth defects, so women taking the medicine have to be sure they don’t get pregnant during treatment.
Possible side effects include:
- Bone or joint pain and difficulty moving
- Red, itchy, burning eyes or other signs your eyes are inflamed
- Nosebleeds
- Red, scaly, burning lips from inflammation
- Skin infection or rash
Additional side effects — rare but still possible — may include:
- Depression
- Suicidal thoughts
- Stomach pain and nausea
- Severe diarrhea
Women who have cystic acne also have these oral medication options:
- Oral contraceptives. Oral contraceptives can be helpful in treating severe acne because of the role hormones play. You may be given birth control pills and an antibiotic or another medicine, spironolactone.
- Sprionolactone, an anti-androgen agent. This prescription medication is used as an alternative treatment for women with severe acne and appears to work quite well. It works by reducing excess oil. However, like isotretinoin, it has side effects including irregular menstruation, urinary frequency, dizziness, headaches, nausea, vomiting, breast tenderness, breast enlargement and an increased risk of developing estrogen-sensitive cancers.
Other Therapies
- Phototherapy therapy. Phototherapy, which uses a light source, may decrease the number of acne-causing bacteria on your skin. An advantage is that light therapy has only minimal side effects, such as dry skin. The light source can be blue light, which does not use ultraviolet light, and won’t damage your skin, or pulsed light and heat energy, which combines light and heat therapy. Like phototherapy, it works by destroying acne-causing bacteria but it also shrinks the glands that make oil.
- Extraction cyst removal. Another treatment option is to remove any large cysts that have formed. One way is for your dermatologist to inject the cyst with a corticosteroid, which will help reduce the size of the cyst and make it less painful. A large, painful acne cyst that medicine doesn’t clear also can be incised and drained. However, do not try this yourself. You risk infection if it’s not done under a doctor’s care.
- Steroid injections. You may benefit from having steroids injected directly into your nodular and cystic lesions. You are likely to see rapid improvement and have less pain. A possible side effect of this treatment: skin thinning in the area that has been injected.
- Chemical peel. A chemical solution made with salicylic, glycolic or retinoic acid, is applied to your skin. However, improvement may not last long and the treatment often needs to be repeated.
3 keys to treatment success
- No matter what treatment you choose, you must give it time to work. It may take up to three months before you see improvement, the AAD says.
- Take your medication as directed. You need to use it properly for it to be most effective.
- Before you take any medication, but especially hormone therapy for your acne, be sure to talk to your dermatologist about any medical conditions you may have, including high blood pressure, heart disease, migraines or cancer.
Bottom line
If you have cystic acne, one of the most severe types of acne, you may just feel like hiding. But remember that you can get help from a dermatologist that will make you proud to show your face in public. Then, to prevent a recurrence:
- Talk to your doctor about whether you need to continue the treatment that cleared your skin or make changes to it. Your cystic acne could return — and quickly— without any treatment.
- Take good care of your skin. Wash your face with a gentle cleanser twice a day. Don’t use anything abrasive (cleanser or scrubber) as that could irritate your skin and make it look worse.
- Wash your hair regularly, especially if it’s oily.
- Think "hands off." If you keep touching your face, you could trigger flares.
- Reduce stress as stress is often a trigger for flares.
Article references
- Who gets acne? National Institute of Arthritis & Musculoskeletal & Skin Diseases. https://www.niams.nih.gov/health-topics/acne#tab-risk
- Acne. National Institute of Arthritis & Musculoskeletal & Skin Diseases. https://www.niams.nih.gov/health-topics/acne#tab-types
- Cyst. The American Academy of Dermatology. https://www.aad.org/teach-healthy-habits/dictionary
- Acne. Girls health.gov. https://www.girlshealth.gov/body/grooming/acne.html
- Acne. Cystic on the face. National Institutes of Health. https://medlineplus.gov/ency/imagepages/2356.htm
- Acne. Cystic on the chest. National Institutes of Health. https://medlineplus.gov/ency/imagepages/2355.htm
- What can clear severe acne? The American Academy of Dermatology Association. https://www.aad.org/severe-acne
- Isotretinoin: The American Academy of Dermatology Association. https://www.aad.org/isotretinoin
- Acne Vulgaris. MSD Manual Professional Version. https://www.msdmanuals.com/professional/dermatologic-disorders/acne-and-related-disorders/acne-vulgaris
- What is acne? National Institutes of Health. https://www.niams.nih.gov/health-topics/acne
- Acne, Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/acne/symptoms-causes/syc-20368047
- Isotretinoin, The Mayo Clinic. https://www.mayoclinic.org/drugs-supplements/isotretinoin-oral-route/side-effects/drg-20068178
- Spironolactone for the treatment of acne in women, a retrospective study of 110 patients. International Journal of Women’s Dermatology, June 2017. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5440451/
- Acne: Tips for Managing, AAD. https://www.aad.org/self-care
- Stubborn Acne? Hormonal Therapy May Help, AAD. https://www.aad.org/hormonal-therapy
- Acne, Johns Hopkins Medicine https://www.hopkinsmedicine.org/health/conditions-and-diseases/acne