Endometriosis Diet: Are There Foods to Eat or Avoid?

While there’s no specific one-size-fits-all diet to definitively alleviate the symptoms of endometriosis, what you eat — and, importantly, what you don’t eat — may have a positive impact on your endometriosis symptoms, namely painful menstrual cramps, pain during or after sex, abdominal pain, heavy menstrual flow and bleeding between periods.
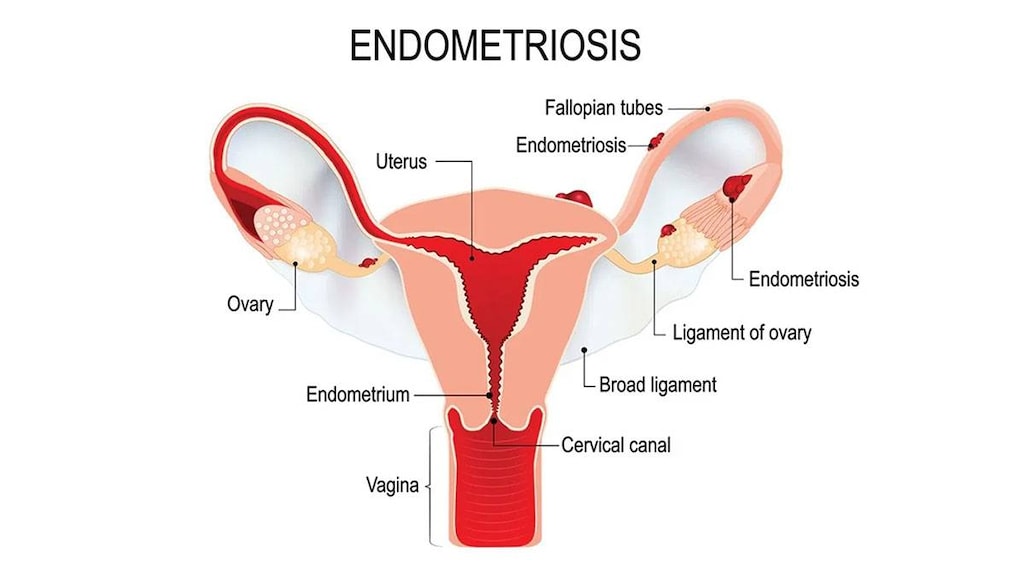
Endometriosis, a painful and common condition, occurs when tissue similar to the endometrium, the lining of the uterus, grows outside of your uterus. It strikes 1 in 10 women of reproductive age and is most often diagnosed in women in their 30s and 40s.
Endometriosis symptoms are often based on where the out-of-place tissue is located. For example, you may experience pain during urination if endometriosis affects your bladder, while constipation and diarrhea may occur if the tissue is near your abdomen. Pain with bowel movements (usually around the time of your period) can also occur if the errant endometrial tissue is near the colon or rectum.
The affected tissue can swell and bleed just as the lining inside of your uterus does every month when you menstruate. With endometriosis, this blood has nowhere to go. Blocked blood can cause inflammation, irritation and scarring. About 40 percent of women with endometriosis will experience infertility because the condition can result in the formation of scar tissue and adhesions throughout the pelvic area.
Before you begin to make any tweaks to your diet, see your doctor for a proper diagnosis. This is important because there are many causes of pelvic pain besides endometriosis.
Your doctor will perform a thorough physical exam and ask questions about your medical history. You will likely also undergo imaging tests of your pelvic region. The only way to diagnose endometriosis with certainty is via a procedure known as a laparoscopy. During this procedure, your doctor inserts a thin tube with a camera and light through a small incision in the abdomen to get a better view of the tissue in question and your pelvic organs. The doctor may also take a biopsy, or small sample, of the tissue.
Treatment for endometriosis often includes over-the-counter non-steroidal anti-inflammatory drugs (NSAIDs) and extended or continuous cycle contraceptives that reduce or eliminate your monthly periods, relieving bleeding. If medications are not effective, surgery can be done to remove the growths, relieve pain and improve your chances of getting pregnant and going full-term.
What to eat
Although medication and surgery are the treatment mainstays for endometriosis, diet can play a role. It’s not just what you include in your diet, but what foods you avoid that may make a difference in your endometriosis symptoms.
However, what you should eat if you have or are at risk for endometriosis includes:
- Fatty fish. Omega-3 fatty acids are known for their anti-inflammatory benefits and can be found in abundance in fatty fish like salmon, tuna and pollock. Omega-3 fatty acids may stave off endometriosis, according to a review published in the Brazilian journal Revista da Associacao Medica Brasileira. The American Heart Association (AHA) recommends that people eat fatty fish at least twice a week to protect against inflammation in general, which can also be a factor in heart disease. Other foods rich in omega-3s include chia seeds, flaxseeds and walnuts, according to the National Institutes of Health. Add more omega-3s in your diet to see if it helps with your endometriosis symptoms.
- Vitamin D. Vitamin D deficiency has been linked to a host of conditions such as the brittle bone disease osteoporosis, heart disease, certain cancers, diabetes, Alzheimer's disease, schizophrenia and possibly endometriosis. Research involving a small trial and published in Gynecological Endocrinology found that women with the lowest blood concentrations of vitamin D also had more severe endometriosis in their ovaries. The findings raise the possibility that vitamin D supplements might improve endometriosis and its symptoms. Your body produces vitamin D when your skin is exposed to sunlight, but to make up for people's shortfalls, it has been added to milk and other foods. Ask your doctor about whether you could be deficient (it takes a simple blood test to find out) or could benefit from taking vitamin D supplements or adding more low-fat dairy foods in your diet.
- Other healthy foods. Green veggies (especially broccoli, kale and spinach), fruits and whole grains (such as brown rice, whole-wheat pasta, bulgur and barley) are important building blocks of a healthy eating plan and can help you maintain a normal weight. As such, they may have positive effects on endometriosis. Make sure your diet includes ample amounts of these important foods.
What not to eat
Foods that are considered inflammatory or are known to raise estrogen levels are among those that you may want to avoid if you have endometriosis. These include:
- Red meat. One large-scale study of nurses published in the American Journal of Obstetrics and Gynecology found that eating both processed and unprocessed red meat ups the risk for developing endometriosis. Red meat is known to be inflammatory, which may affect endometriosis symptoms. In addition, red meat is high in saturated fat, which is linked to weight gain. Choose lean sources of protein, such as chicken and fish, instead of red meat.
- Gluten. Gluten is the umbrella term for proteins in wheat, rye, barley and triticale (a cross between wheat and rye). Gluten may worsen inflammation in some women. In fact, one study in the European journal Minerva Chirurgica found that 75 percent of women who eliminated gluten from their diets for one year reported a decrease in pelvic pain. What’s more, everyone in the study reported that they felt better physically and mentally after eliminating gluten from their diets.
Is the FODMAP diet the answer?
FODMAP stands for fermentable oligosaccharides, disaccharides, monosaccharides and polyols — components in certain carb-based foods that, for some people, are poorly absorbed in the intestines, according to the Cleveland Clinic. They can feed bad bacteria in your gut and cause gas, abdominal pain, diarrhea or constipation, which may worsen symptoms of endometriosis.
One category of high-FODMAP foods is dairy, mostly because of the lactose found in milk, cottage cheese, cream cheese, ice cream and sour cream. Others include high-fructose fruits, like apples and pears, and cruciferous vegetables, like brussel sprouts and cabbage. And yes, these are foods that are otherwise considered healthy. A low-FODMAP diet, which has been suggested for people with irritable bowel syndrome (IBS), may also help with endometriosis, according to a study published in Obstetrics & Gynecology. It found that women with endometriosis and IBS who ate a low-FODMAP diet for one year had an even greater reduction in symptoms (72 percent) than did the women with IBS alone (49 percent).
Talk to your doctor about trying a low-FODMAP diet to see if it affects your endometriosis symptoms. Your doctor may also suggest low-FODMAP substitutes for some of your dietary staples.
Breaking the endometriosis-estrogen connection
Keeping estrogen levels low may help diminish your chance of developing endometriosis. The female sex hormone estrogen helps to thicken the lining of your uterus during your menstrual cycle and may feed or fuel endometriosis as a result.
Alcohol is known to raise estrogen levels, so keeping your consumption to a minimum is a smart diet strategy. In particular, don’t consume more than one drink a day.
Also, skip the 24-ounce large coffee next time you go to your favorite coffee shop. Drinking more than one caffeinated drink a day — and that includes bad-for-you sodas and good-for-you green tea — can raise estrogen levels. The upper daily limit for caffeine is 400 milligrams (mg). Just one 8-ounce cup of coffee may have as many as 165 mg. To keep estrogen levels down, also try to exercise more than 4 hours a week and maintain a low percentage of body fat.
One final tip
When it comes to using diet to improve endometriosis symptoms, it’s important to keep a food log. Detail everything you can, both the foods you are avoiding and those you’re increasing along with any symptoms and changes in symptoms that you experience. Your diary should shed light on patterns that will help you tweak your diet. Share this information with your doctor or a registered dietitian to make sure that you are eating a healthy well-rounded diet.
Article references
- American College of Obstetricians and Gynecologists, Endometriosis - https://www.acog.org/Patients/FAQs/Endometriosis
- Mayo Clinic, Endometriosis Diagnosis and Treatment - https://www.mayoclinic.org/diseases-conditions/endometriosis/diagnosis-treatment/drc-20354661
- Resolve, Endometriosis - https://resolve.org/infertility-101/medical-conditions/endometriosis/
- Revista da Associacao Medica Brasileira, “Nutritional aspects related to endometriosis” - http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0104-42302015000600519&lng=en&nrm=iso&tlng=en
- American Heart Association, Fish and Omega 3 Fatty Acids - http://www.heart.org/HEARTORG/GettingHealthy/NutritionCenter/HealthyDietGoals/Fish-and-Omega-3-Fatty-Acids_UCM_303248_Article.jsp
- U.S. National Library of Medicine, Vitamin D deficiency - https://medlineplus.gov/vitaminddeficiency.html
- Gynecological Endocrinology, “Ovarian endometriosis and vitamin D serum levels” - https://www.tandfonline.com/doi/full/10.1080/09513590.2016.1239254
- American Journal of Obstetrics and Gynecology, “A prospective cohort study of meat and fish consumption and endometriosis risk” - https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6066416/
- Academy of Nutrition and Dietetics, Healthy eating for women - https://www.eatright.org/food/nutrition/dietary-guidelines-and-myplate/healthy-eating-for-women
- Minerva Chirurgica, Gluten-free diet: a new strategy for management of painful endometriosis related symptoms? - http://europepmc.org/article/med/23334113
- Obstetrics & Gynecology, Endometriosis in patients with irritable bowel syndrome: Specific symptomatic and demographic profile, and response to the low FODMAP diet - https://obgyn.onlinelibrary.wiley.com/doi/abs/10.1111/ajo.12594
- Cleveland Clinic, Take Control of IBS with Low FODMAP diet - https://health.clevelandclinic.org/take-control-of-ibs-with-low-fodmap-diet/
- Office on Women's Health, Endometriosis - https://www.womenshealth.gov/a-z-topics/endometriosis
- Mayo Clinic, Caffeine - https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/caffeine/art-20049372?p=1
- National Institutes of Health, Omega-3 fatty acids - https://ods.od.nih.gov/factsheets/Omega3FattyAcids-Consumer/
- St. Louis University, The Anti-Inflammation and Elimination Diet for Adults Living With Endometriosis - http://obgyn.slu.edu/uploads/centerforendo/Combined%20Anti-Inflammatory%20and%20Elimination%20Diet%20for%20Adults%20Living%20with%20Endometriosis%20booklet.pdf