Understanding Endometriosis Pain

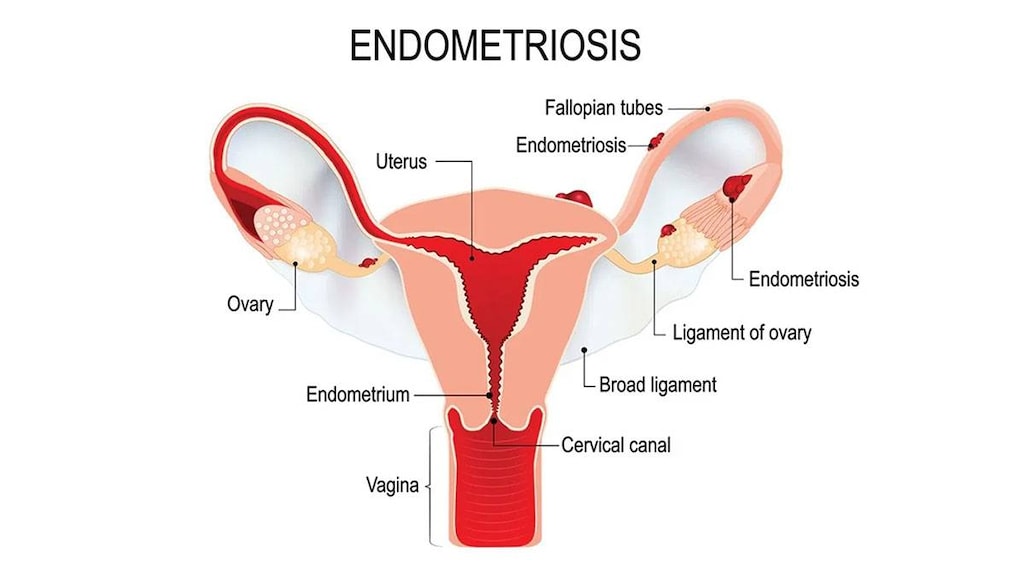
Endometriosis is a fairly common health condition that happens when tissue that's similar to the tissue that normally lines the inside of the uterus starts growing outside the uterus, on parts of your body where it should not be. This causes growths that can swell and bleed and cause pain during menstruation as the growths become trapped because there is no way for the tissue to leave the body. Endometriosis growths can cause ovarian cysts, scar tissue that can make it more difficult to conceive, and can lead to adhesions that stick tissue and organs together.
Endometriosis most often affects the ovaries, fallopian tubes and parts of the uterus, but the growths can also occur in the vagina, rectum, cervix, vulva, bladder and bowel. Though rare, it also can affect the brain, lungs and skin, notes the U.S. Office on Women's Health, part of the Department of Health and Human Services (HHS).
Treatments for endometriosis include medication and surgery. A correct diagnosis is important for proper treatment, especially because the signs and symptoms of endometriosis are sometimes confused with those of other conditions.
Endometriosis most often develops in women in their 30s and 40s, and affects more than 11 percent of American women 15 to 44 years old, according to HHS.
Menstrual pain or endometriosis?
Many women experience menstrual pain or cramps during their monthly cycle, so how can you tell if that’s normal period pain or endometriosis pain? The Mayo Clinic notes that endometriosis is often much more severe and the pain can increase over time (from month-to-month and over years), compared with regular menstrual pain. Other symptoms of endometriosis include:
- Heavy bleeding. Those with endometriosis may have very heavy periods or bleeding between periods.
- Pain. Lower back pain and strong pelvic and abdominal pain may occur before you start your period or last throughout your period. Additionally, you may feel pain when you go to the bathroom during your menstrual cycle - pain that can be felt when you pass urine or have a bowel movement. A woman may also feel pain during sex.
- Infertility. For women who are trying to get pregnant without success, endometriosis may be to blame.
- Not feeling well. Symptoms like nausea, bloating, constipation, diarrhea or feeling very tired are common symptoms of endometriosis.
Diagnosing endometriosis
It’s important for women who are suffering from painful periods or who think they may have endometriosis to be correctly diagnosed. How is this done? Your doctor may do a full pelvic exam to feel for cysts or scars around the uterus (although small areas of scarring will not be felt on examination). You may also have an ultrasound or MRI to show the doctor what's happening inside your pelvic area. Additionally, your doctor may suggest that you have a procedure called a laparoscopy, in which a small scope is inserted in your pelvic/abdominal area so the doctor can detect any signs of endometriosis.
Treating endometriosis and managing the pain
While there is no cure for endometriosis, a variety of treatment options are available. Not every option works for every woman, so your doctor may try a few different routes. Before deciding on a treatment option, your doctor will factor in a few elements, including the intensity of your pain, your age and if you’re trying to get pregnant or want children at some point.
Pain Medication
According to the National Institutes of Health (NIH), the first option your doctor may have you try is pain medication. This is often given to women who have mild pain, and the medication may be over-the-counter or by prescription. The most common over-the-counter pain medications are NSAIDs (non-steroidal anti-inflammatory drugs), such as ibuprofen (Motrin, Advil) and narpoxen (Aleve). When using NSAIDs, NIH notes that women should not use them longer than 10 days for treating pain — unless specifically instructed to do so by your doctor — because these medications are meant for short-term use and can have side effects.
Hormone Treatments
Hormone treatments are another option your doctor may suggest to treat pain from endometriosis. While hormone treatments can’t make existing adhesions disappear, they can be effective in preventing or slowing the growth of new scars. What’s happening is that the hormone treatments work in such a way that your body stops producing estrogen and/or progestin. This helps slow both the endometrial tissue growth and prevent new implants of endometrial tissue.
Birth control pills, patches and vaginal rings may be given to women who are not trying to get pregnant. The benefits of these hormonal contraceptives include lighter periods, less painful periods and a more regular and shorter menstrual cycle.
Another hormone treatment that your doctor may recommend is progesterone and progestin, which can be prescribed in various ways: as an intrauterine device (IUD) with levonorgestrel, as a pill that you take daily, as a contraceptive implant that can last up to four years or as a contraceptive shot given every three months. All of these methods prevent pregnancy.
Other possible hormone treatment options include the drug danazol, a hormone similar to testosterone that works to decrease the amount of hormone made in the ovaries. This medication has many side effects, and its use has declined after the introduction of gonadotropin-releasing hormone (GnRH) agonists/antagonists.
GnRH agonists/antagonists block the production of ovarian-stimulating hormones, lowering estrogen levels. This will put your body into a state of menopause because it prevents ovulation and menstruation. Women are often advised to take a low dose of estrogen or progestin when taking this type of medication to decrease menopausal side effects, such as hot flashes, vaginal dryness and bone loss.
Surgery
Surgery is often a last resort, used if symptoms are severe, if your body is not responding to over-the-counter medications or hormone therapy or if you’re trying to get pregnant.
The surgical procedure may involve removing the lesions (called excising) or destroying the lesions via extreme heat (called cauterizing). The doctor may also remove scar tissue.
The goal of surgery is to keep healthy tissue intact, but remove the endometriosis.
Pregnancy, menopause and endometriosis
Women may think they can’t get pregnant if they have endometriosis, but that's not true. However, it may be harder to get pregnant. Some researchers, in fact, think that about half of women with infertility issues may have endometriosis. Some believe that this is because the endometrium, which is where implantation of the egg takes place, has not developed properly. Others think that the immune system — which is supposed to defend the body against harmful diseases and substances — instead may be attacking the embryo. Still others think that endometriosis makes it hard for the sperm to find the egg because the endometriosis is blocking the reproductive organs.
As for menopause, women in this stage of life no longer make the hormone estrogen. That means that endometriosis growths may reduce in size, and the pain may subside. However, if a woman is taking menopausal hormone therapy, she may still have the symptoms, including pain.
The bottom line
While any female can develop endometriosis, certain risk factors may make you more susceptible, according to HHS. These include:
- Not having had children
- Having periods that last longer than seven days
- Having periods that occur more often than every 27 days
- Having a sister, mother or aunt with the condition
- Having another health problem that affects the flow of blood during your period
If you have these risk factors, or if you're suffering from painful periods or having a hard time getting pregnant, talk with your doctor about whether endometriosis might be involved. Though HHS notes that you cannot prevent endometriosis, a variety of treatment options do exist for painful periods and fertility issues related to endometriosis.
Article references
- Mayo Clinic, Endometriosis https://www.mayoclinic.org/diseases-conditions/endometriosis/symptoms-causes/syc-20354656
- NICHD, Endometriosis Treatment https://www.nichd.nih.gov/health/topics/endometri/conditioninfo/treatment
- Cleveland Clinic, NSAIDs https://my.clevelandclinic.org/health/drugs/11086-non-steroidal-anti-inflammatory- medicines-nsaids
- Cleveland Clinic, Endometriosis: Diagnosis and Tests https://my.clevelandclinic.org/health/diseases/10857-endometriosis/diagnosis-and-tests
- U.S. Department of Health and Human Services, Endometriosis https://www.womenshealth.gov/a-z-topics/endometriosis