Ascariasis (as-kuh-RIE-uh-sis) is a type of roundworm infection. These worms are parasites that use your body as a host to mature from larvae or eggs to adult worms. Adult worms, which reproduce, can be more than a foot (30 centimeters) long.
One of the most common worm infections in people worldwide, ascariasis is uncommon in the United States. Most infected people have mild cases with no symptoms. But heavy infestation can lead to serious symptoms and complications.
Ascariasis occurs most often in children in tropical and subtropical regions of the world — especially in areas with poor sanitation and hygiene.
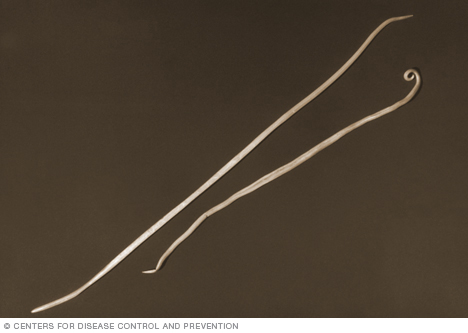
Ascariasis worms are typically pink or white with tapered ends. Female worms can be more than 15 inches (40 centimeters) long and a little less than a quarter inch (6 millimeters) in diameter. Male worms are generally smaller.
Symptoms
Most people infected with ascariasis have no signs or symptoms. Moderate to heavy infestations cause various signs or symptoms, depending on which part of your body is affected.
In the lungs
After you swallow the tiny (microscopic) ascariasis eggs, they hatch in the small intestine and the larvae migrate through the bloodstream or lymphatic system into the lungs. At this stage, you may experience signs and symptoms similar to asthma or pneumonia, including:
- Persistent cough
- Shortness of breath
- Wheezing
After spending 10 to 14 days in the lungs, the larvae travel to the throat, where you cough them up and then swallow them.
In the intestines
The larvae mature into adult worms in the small intestine, and the adult worms typically live in the intestines until they die. In mild or moderate ascariasis, the intestinal infestation can cause:
- Vague abdominal pain
- Nausea and vomiting
- Diarrhea or bloody stools
If you have a large number of worms in the intestine, you might have:
- Severe abdominal pain
- Fatigue
- Vomiting
- Weight loss or malnutrition
- A worm in your vomit or stool
When to see a doctor
Talk to your doctor if you have persistent abdominal pain, diarrhea or nausea.
Causes
Ascariasis isn't spread directly from person to person. Instead, a person has to come into contact with soil mixed with human or pig feces that contain ascariasis eggs or infected water. In some developing countries, human feces are used for fertilizer, or poor sanitary facilities allow human waste to mix with soil in yards, ditches and fields. People can also get it from eating uncooked pig or chicken liver that is infected.
Small children often play in dirt, and infection can occur if they put their dirty fingers in their mouths. Unwashed fruits or vegetables grown in contaminated soil also can transmit the ascariasis eggs.
Life cycle of a worm
- Ingestion. The tiny (microscopic) ascariasis eggs can't become infective without coming into contact with soil. People can accidentally ingest (swallow) contaminated soil through hand-to-mouth contact or by eating uncooked fruits or vegetables that have been grown in contaminated soil.
- Migration. Larvae hatch from the eggs in your small intestine and then go through the intestinal wall to travel to the heart and lungs via the bloodstream or lymphatic system. After maturing for about 10 to 14 days in your lungs, the larvae break into your airway and travel up the throat, where they're coughed up and swallowed.
- Maturation. Once they're back in the intestines, the parasites grow into male or female worms. Female worms can be more than 15 inches (40 centimeters) long and a little less than a quarter inch (6 millimeters) in diameter. Male worms are generally smaller.
- Reproduction. Female worms can produce 200,000 eggs a day if there are both female and male worms in the intestines, and the eggs leave your body in feces. The fertilized eggs must be in soil for at least two to four weeks before they become infective.
The whole process — from egg ingestion to egg deposits — takes about two or three months. Ascariasis worms can live inside your body for a year or two.
Risk factors
Risk factors for ascariasis include:
- Age. Most people who have ascariasis are 10 years old or younger. Children in this age group may be at higher risk because they're more likely to play in dirt.
- Warm climate. In the United States, ascariasis is more common in the Southeast. But it's more frequent in developing countries with warm temperatures year-round.
- Poor sanitation. Ascariasis is widespread in developing countries where human feces are allowed to mix with local soil.
Complications
Mild cases of ascariasis usually don't cause complications. If you have a heavy infestation, potentially dangerous complications may include:
- Slowed growth. Loss of appetite and poor absorption of digested foods put children with ascariasis at risk of not getting enough nutrition, which can slow growth.
- Intestinal blockage and perforation. In heavy ascariasis infestation, a mass of worms can block a portion of your intestine. This can cause severe abdominal cramping and vomiting. The blockage can even make a hole in the intestinal wall or appendix, causing internal bleeding (hemorrhage) or appendicitis.
- Duct blockages. In some cases, worms may block the narrow ducts of your liver or pancreas, causing severe pain.
Prevention
The best defense against ascariasis is good hygiene and common sense. Follow these tips to avoid infection:
- Practice good hygiene. Before handling food, always wash your hands with soap and water. Wash fresh fruits and vegetables thoroughly.
- Use care when traveling. Use only bottled water, and avoid raw vegetables unless you can peel and wash them.
Diagnosis
To diagnose ascariasis, your doctor may review your symptoms and order tests.
In heavy infestations, it's possible to find worms after you cough or vomit. The worms can come out of other body openings, such as your mouth or nostrils. If this happens to you, take the worm to your doctor so that he or she can identify it and prescribe the proper treatment.
Stool tests
Mature female ascariasis worms in your intestine begin laying eggs. These eggs travel through your digestive system and eventually can be found in your stool.
To diagnose ascariasis, your doctor will examine your stool for the tiny (microscopic) eggs and larvae. But eggs won't appear in stool until at least 40 days after you're infected. And if you're infected with only male worms, you won't have eggs.
Blood tests
Your blood can be tested for the presence of an increased number of a certain type of white blood cell, called eosinophils. Ascariasis can elevate your eosinophils, but so can other types of health problems.
Imaging tests
- X-rays. If you're infested with worms, the mass of worms may be visible in an X-ray of the abdomen. In some cases, a chest X-ray can reveal the larvae in the lungs.
- Ultrasound. An ultrasound may show worms in the pancreas or liver. This technology uses sound waves to create images of internal organs.
- CT scans or MRIs. Both types of tests create detailed images of the internal structures, which can help your doctor detect worms that are blocking ducts in the liver or pancreas. CT scans combine X-ray images taken from many angles. MRI uses radio waves and a strong magnetic field.
Treatment
Typically, only infections that cause symptoms need to be treated. In some cases, ascariasis will resolve on its own.
Medications
Anti-parasite medications are the first line of treatment against ascariasis. The most common are:
- Albendazole (Albenza)
- Ivermectin (Stromectol)
- Mebendazole
These medications, taken for one to three days, kill the adult worms. Side effects include mild abdominal pain or diarrhea.
Pregnant women may take pyrantel pamoate.
Surgery
In cases of heavy infestation, surgery may be necessary to remove worms and repair damage they've caused. Intestinal blockage or holes, bile duct blockage, and appendicitis are complications that may require surgery.
Preparing for an appointment
Your family doctor might refer you to a doctor trained in digestive disorders (gastroenterologist). You may need to see a surgeon if the worms have blocked the intestines.
What you can do
Before your appointment, you may want to write down the answers to the following questions:
- When did your symptoms begin?
- Does anything make your symptoms better or worse?
- Have you noticed worms in your stool or vomit?
- Have you traveled to developing countries lately?
- What medications and supplements are you taking?
What to expect from your doctor
During the physical exam, your doctor may press on certain areas of the abdomen to check for pain or tenderness. He or she may also want a sample of stool for testing.
Copyright © 1998-2026 Mayo Foundation for Medical Education and Research (MFMER). All rights reserved.