Boxed Warning
Lactic acidosis:
Postmarketing cases of metformin-associated lactic acidosis have resulted in death, hypothermia, hypotension, and resistant bradyarrhythmias. The onset of metformin-associated lactic acidosis is often subtle, accompanied only by nonspecific symptoms, such as malaise, myalgias, respiratory distress, somnolence, and abdominal pain. Metformin-associated lactic acidosis was characterized by elevated blood lactate levels (>5 mmol/L), anion gap acidosis (without evidence of ketonuria or ketonemia), an increased lactate/pyruvate ratio; and metformin plasma levels generally >5 mcg/mL.
Risk factors for metformin-associated lactic acidosis include renal impairment, concomitant use of certain drugs (eg, carbonic anhydrase inhibitors such as topiramate), age 65 years or older, having a radiological study with contrast, surgery and other procedures, hypoxic states (eg, acute congestive heart failure), excessive alcohol intake, and hepatic impairment.
Steps to reduce the risk of and manage metformin-associated lactic acidosis in these high risk groups are provided in the full prescribing information.
If metformin-associated lactic acidosis is suspected, immediately discontinue alogliptin and metformin and institute general supportive measures in a hospital setting. Prompt hemodialysis is recommended.
Dosage Forms
Excipient information presented when available (limited, particularly for generics); consult specific product labeling.
Tablet, Oral:
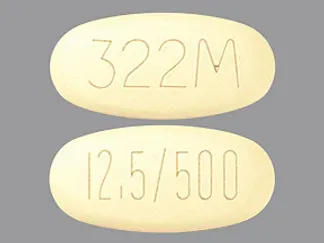
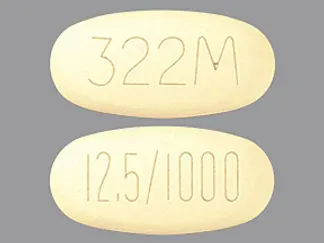
Kazano: Alogliptin 12.5 mg and metformin hydrochloride 500 mg, Alogliptin 12.5 mg and metformin hydrochloride 1000 mg
Generic: Alogliptin 12.5 mg and metformin hydrochloride 1000 mg, Alogliptin 12.5 mg and metformin hydrochloride 500 mg
Pharmacology
Mechanism of Action
Alogliptin inhibits dipeptidyl peptidase 4 (DPP-4) enzyme resulting in prolonged active incretin levels. Incretin hormones (eg, glucagon-like peptide-1 [GLP-1] and glucose-dependent insulinotropic polypeptide [GIP]) regulate glucose homeostasis by increasing insulin synthesis and release from pancreatic beta cells and decreasing glucagon secretion from pancreatic alpha cells. Decreased glucagon secretion results in decreased hepatic glucose production. Under normal physiologic circumstances, incretin hormones are released by the intestine throughout the day and levels are increased in response to a meal; incretin hormones are rapidly inactivated by the DPP-4 enzyme.
Metformin decreases hepatic glucose production, decreasing intestinal absorption of glucose, and improves insulin sensitivity (increases peripheral glucose uptake and utilization).
Use: Labeled Indications
Diabetes mellitus, type 2: As an adjunct to diet and exercise to improve glycemic control in adults with type 2 diabetes mellitus when treatment with both alogliptin and metformin is appropriate as monotherapy or combination therapy.
Contraindications
Serious hypersensitivity (eg, anaphylaxis, angioedema, severe dermatologic reactions) to products that contain alogliptin, metformin, or any component of the formulation; severe renal impairment (eGFR <30 mL/minute/1.73 m2); acute or chronic metabolic acidosis including diabetic ketoacidosis
Canadian labeling: Additional contraindications (not in US labeling): Unstable and/or insulin-dependent (type 1) diabetes mellitus; history of ketoacidosis with or without coma; history of lactic acidosis (regardless of precipitating factors); unknown renal function; renal disease or renal dysfunction (serum creatinine above upper limit of normal or CrCl <60 mL/minute), which may also result from conditions such as cardiovascular collapse, acute myocardial infarction, and septicemia; excessive alcohol intake, acute or chronic; severe hepatic dysfunction; cardiovascular collapse and disease states associated with hypoxemia (eg, cardiorespiratory insufficiency), which are often associated with hyperlactacidemia; stress conditions (eg, severe infections, trauma or surgery and the recovery period); severe dehydration; pregnancy; breast-feeding.
Dosage and Administration
Dosing: Adult
Diabetes mellitus, type 2: Oral: Initial doses should be based on current daily dose of alogliptin and metformin; Range: Alogliptin 12.5 mg/metformin 500 to 1000 mg twice daily. Maximum: Alogliptin 12.5 mg/metformin 1,000 mg twice daily
Concomitant use with insulin or insulin secretagogues: Reduced dose of insulin or insulin secretagogues (eg, sulfonylureas) may be needed.
Dosing: Geriatric
Refer to adult dosing. The initial and maintenance dosing should be conservative, due to the potential for decreased renal function (monitor).
Administration
Oral: Administer with food. Swallow tablets whole; do not split or divide.
Dietary Considerations
Individualized medical nutrition therapy (MNT) based on ADA recommendations is an integral part of therapy. Monitor for signs and symptoms of vitamin B12 and/or folic acid deficiency; supplementation may be required.
Storage
Store at 25°C (77°F); excursions permitted to 15°C to 30°C (59°F to 86°F). Protect from moisture.
Alogliptin and Metformin Images
Drug Interactions
Abemaciclib: May increase the serum concentration of MetFORMIN. Monitor therapy
Alcohol (Ethyl): May enhance the adverse/toxic effect of MetFORMIN. Specifically, alcohol may potentiate the risk of lactic acidosis Avoid combination
Alpha-Lipoic Acid: May enhance the hypoglycemic effect of Antidiabetic Agents. Monitor therapy
Androgens: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Exceptions: Danazol. Monitor therapy
Bictegravir: May increase the serum concentration of MetFORMIN. Monitor therapy
Carbonic Anhydrase Inhibitors: May enhance the adverse/toxic effect of MetFORMIN. Specifically, the risk of developing lactic acidosis may be increased. Exceptions: Brinzolamide; Dorzolamide. Monitor therapy
Cephalexin: May increase the serum concentration of MetFORMIN. Monitor therapy
Cimetidine: May increase the serum concentration of MetFORMIN. Management: Consider alternatives to cimetidine in patients receiving metformin due to a potential for increased metformin concentrations and toxicity (including lactic acidosis). Consider therapy modification
Dalfampridine: MetFORMIN may increase the serum concentration of Dalfampridine. Dalfampridine may increase the serum concentration of MetFORMIN. Monitor therapy
Direct Acting Antiviral Agents (HCV): May enhance the hypoglycemic effect of Antidiabetic Agents. Monitor therapy
Dofetilide: MetFORMIN may increase the serum concentration of Dofetilide. Monitor therapy
Dolutegravir: May increase the serum concentration of MetFORMIN. Management: Consider the risks and benefits of this combination. If combined, limit the daily metformin dose to 1,000 mg when used with dolutegravir. Monitor for increased metformin effects/toxicities (including lactic acidosis) during concomitant use. Consider therapy modification
Erdafitinib: May increase the serum concentration of OCT2 Substrates. Monitor therapy
Glycopyrrolate (Systemic): May increase the serum concentration of MetFORMIN. Monitor therapy
Guanethidine: May enhance the hypoglycemic effect of Antidiabetic Agents. Monitor therapy
Hyperglycemia-Associated Agents: May diminish the therapeutic effect of Antidiabetic Agents. Monitor therapy
Hypoglycemia-Associated Agents: Antidiabetic Agents may enhance the hypoglycemic effect of Hypoglycemia-Associated Agents. Monitor therapy
Insulins: Dipeptidyl Peptidase-IV Inhibitors may enhance the hypoglycemic effect of Insulins. Management: Consider a decrease in insulin dose when initiating therapy with a dipeptidyl peptidase-IV inhibitor and monitor patients for hypoglycemia. Consider therapy modification
Iodinated Contrast Agents: May enhance the adverse/toxic effect of MetFORMIN. Renal dysfunction that may be caused by iodinated contrast agents may lead to metformin-associated lactic acidosis. Management: Management advice varies. Refer to the full drug interaction monograph content for details. Exceptions: Diatrizoate Meglumine; Diatrizoate Sodium; Ethiodized Oil. Consider therapy modification
Isavuconazonium Sulfate: May increase the serum concentration of MetFORMIN. Monitor therapy
LamoTRIgine: May increase the serum concentration of MetFORMIN. Management: The lamotrigine Canadian product monograph states that coadministration of these drugs is not recommended. Monitor therapy
Maitake: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Monitor therapy
Monoamine Oxidase Inhibitors: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Monitor therapy
Nonsteroidal Anti-Inflammatory Agents: May enhance the adverse/toxic effect of MetFORMIN. Monitor therapy
Ombitasvir, Paritaprevir, and Ritonavir: May enhance the adverse/toxic effect of MetFORMIN. Specifically, the risk for lactic acidosis may be increased. Monitor therapy
Ombitasvir, Paritaprevir, Ritonavir, and Dasabuvir: May enhance the adverse/toxic effect of MetFORMIN. Specifically, the risk for lactic acidosis may be increased. Monitor therapy
Ondansetron: May increase the serum concentration of MetFORMIN. Monitor therapy
Patiromer: May decrease the serum concentration of MetFORMIN. Management: Administer metformin at least 3 hours before or 3 hours after patiromer. Consider therapy modification
Pegvisomant: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Monitor therapy
Prothionamide: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Monitor therapy
Quinolones: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Quinolones may diminish the therapeutic effect of Blood Glucose Lowering Agents. Specifically, if an agent is being used to treat diabetes, loss of blood sugar control may occur with quinolone use. Monitor therapy
Ranolazine: May increase the serum concentration of MetFORMIN. Management: Limit the metformin dose to a maximum of 1,700 mg per day when used together with ranolazine 1,000 mg twice daily. Monitor patients for metformin toxicities, including lactic acidosis and carefully weigh the risks and benefits of this combination. Consider therapy modification
Ritodrine: May diminish the therapeutic effect of Antidiabetic Agents. Monitor therapy
Salicylates: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Monitor therapy
Selective Serotonin Reuptake Inhibitors: May enhance the hypoglycemic effect of Blood Glucose Lowering Agents. Monitor therapy
Sulfonylureas: Dipeptidyl Peptidase-IV Inhibitors may enhance the hypoglycemic effect of Sulfonylureas. Management: Consider a decrease in sulfonylurea dose when initiating therapy with a dipeptidyl peptidase-IV inhibitor and monitor patients for hypoglycemia. Consider therapy modification
Tafenoquine: May increase the serum concentration of MATE1 Substrates. Management: Avoid use of MATE substrates with tafenoquine, and if the combination cannot be avoided, monitor closely for evidence of toxicity of the MATE substrate and consider a reduced dose of the MATE substrate according to that substrate's labeling. Consider therapy modification
Tafenoquine: May increase the serum concentration of OCT2 Substrates. Management: Avoid use of OCT2 substrates with tafenoquine, and if the combination cannot be avoided, monitor closely for evidence of toxicity of the OCT2 substrate and consider a reduced dose of the OCT2 substrate according to that substrate's labeling. Consider therapy modification
Thiazide and Thiazide-Like Diuretics: May diminish the therapeutic effect of Antidiabetic Agents. Monitor therapy
Topiramate: May enhance the adverse/toxic effect of MetFORMIN. Monitor therapy
Trimethoprim: May increase the serum concentration of MetFORMIN. Monitor therapy
Trospium: MetFORMIN may decrease the serum concentration of Trospium. Monitor therapy
Vandetanib: May increase the serum concentration of MetFORMIN. Monitor therapy
Verapamil: May diminish the therapeutic effect of MetFORMIN. Monitor therapy
Adverse Reactions
Percentages as reported with combination product. Also see individual agents.
1% to 10%:
Central nervous system: Headache (5%)
Endocrine & metabolic: Hypoglycemia (2% to 5%)
Gastrointestinal: Diarrhea (6%)
Genitourinary: Urinary tract infection (4%)
Neuromuscular & skeletal: Back pain (4%)
Respiratory: Upper respiratory tract infection (8%), nasopharyngitis (7%)
<1%, postmarketing, and/or case reports: Severe arthralgia (FDA Safety Alert, Aug 28, 2015)
Warnings/Precautions
Concerns related to adverse effects:
- Arthralgia: Severe and disabling arthralgia has been reported with DPP-4 inhibitor use; onset may occur within one day to years after treatment initiation and may resolve with discontinuation of therapy. Some patients may experience a recurrence of symptoms if DPP-4 inhibitor therapy resumed. Discontinue use if severe joint pain results from DPP-4 inhibitor therapy.
- Bullous pemphigoid: DPP-4 inhibitor use has been associated with development of bullous pemphigoid; cases have typically resolved with topical or systemic immunosuppressive therapy and discontinuation of DPP-4 inhibitor therapy. Advise patients to report development of blisters or erosions. Discontinue therapy if bullous pemphigoid is suspected and consider referral to a dermatologist.
- Hepatotoxicity: Cases of fatal and non-fatal hepatic failure have been reported in postmarketing surveillance with alogliptin. Baseline liver function tests (serum transaminases) are recommended to rule out underlying liver diseases. Use with caution in patients with abnormal serum transaminases. Monitor and promptly evaluate serum transaminase levels in patients with symptoms of hepatic injury (eg, fatigue, anorexia, jaundice, dark urine, and/or abdominal pain). In patients with clinically significant transaminase elevations and/or persistent or worsening elevations, therapy should be interrupted. Therapy should only be resumed with caution in patients where an alternative cause of transaminase elevations has been determined.
- Hypersensitivity reactions: Rare hypersensitivity reactions, including anaphylaxis, angioedema, and/or severe dermatologic reactions such as Stevens-Johnson syndrome, have been reported in postmarketing surveillance with alogliptin; discontinue if signs/symptoms of hypersensitivity reactions occur. Use with caution if patient has experienced angioedema with other DPP-4 inhibitor use.
- Lactic acidosis: [US Boxed Warning]: Postmarketing cases of metformin-associated lactic acidosis have resulted in death, hypothermia, hypotension, and resistant bradyarrhythmias. The onset is often subtle, accompanied by nonspecific symptoms (eg, malaise, myalgias, respiratory distress, somnolence, abdominal pain); elevated blood lactate levels (>5 mmol/L); anion gap acidosis (without evidence of ketonuria or ketonemia); increased lactate:pyruvate ratio; metformin plasma levels generally >5 mcg/mL. Risk factors for lactic acidosis include patients with renal impairment, concomitant use of certain drugs (eg, carbonic anhydrase inhibitors such as topiramate), ≥65 years, having a radiologic study with contrast, surgery and other procedures, hypoxic states (eg, acute heart failure), excessive alcohol intake, and hepatic impairment. Discontinue immediately if lactic acidosis is suspected; prompt hemodialysis is recommended. Lactic acidosis should be suspected in any patient with diabetes receiving metformin with evidence of acidosis but without evidence of ketoacidosis. Discontinue use in patients with conditions associated with dehydration, hypoperfusion, sepsis, or hypoxemia. Temporarily discontinue therapy in patients with restricted food and fluid intake. The risk of accumulation and lactic acidosis increases with the degree of impairment of renal function.
- Pancreatitis: Cases of acute pancreatitis have been reported with alogliptin use. Monitor for signs/symptoms of pancreatitis; discontinue use immediately if pancreatitis is suspected and initiate appropriate management. Use with caution in patients with a history of pancreatitis as it is not known if this population is at greater risk.
- Vitamin B12 concentrations: Long-term metformin use is associated with vitamin B12 deficiency; monitor vitamin B12 serum concentrations periodically with long-term therapy. Monitoring of B12 serum concentrations should be considered in all patients receiving metformin and in particular those with peripheral neuropathy or anemia (ADA 2019).
Disease-related concerns:
- Bariatric surgery:
– Altered absorption: Use individual components of the formulation as IR tablets or solution after surgery. Absorption may be altered given the anatomic and transit changes created by gastric bypass and sleeve gastrectomy surgery. Tablets may have a reduced effect after gastric bypass or sleeve gastrectomy due to the direct bypass of the stomach and proximal small bowel with gastric bypass or a more rapid gastric emptying and proximal small bowel transit with sleeve gastrectomy (Mechanick 2013; Melissas 2013). After gastric bypass (Roux-en-Y gastric bypass [RYGB]), administration of IR tablets led to increased absorption (AUC0-∞ increased by 21%) and bioavailability (increased by 50%) (Padwal 2011). Lactate levels decrease after gastric bypass (RYGB)-induced weight loss irrespective of the use of metformin. Routinely lowering metformin dose after gastric bypass is not necessary as long as normal renal function is preserved (Deden 2018).
– Glucagon-like peptide-1 exposure and therapeutic efficacy: Closely monitor for signs and symptoms of pancreatitis; gastric bypass and sleeve gastrectomy may increase endogenous secretion of glucagon-like peptide-1 (Korner 2009; Peterli 2012). A single-dose, placebo-controlled study evaluated short-term therapy (4 weeks) with sitagliptin in gastric bypass patients having persistent or recurrent type 2 diabetes and found it to be well tolerated and provided a small but significant reduction in postprandial blood glucose (Shah 2018).
- Heart failure: In a multi-center, randomized, double-blind, placebo-controlled cardiovascular outcome trial of patients with type 2 diabetes and recent acute coronary syndrome, the overall incidence of hospitalization for heart failure (HF) was slightly greater in the alogliptin arm compared with placebo (3.9% vs 3.3%), but this difference was not statistically significant. In patients without a history of HF, the incidence of hospitalization for HF was greater with alogliptin than placebo (2.2% vs 1.3%), a difference that reached statistical significance (Zannad 2015). The ADA suggests DPP-4 inhibitors (except saxagliptin) may be considered in patients with HF (ADA 2019). Metformin may be used in patients with stable HF; avoid use in unstable or hospitalized patients with HF (ADA 2019). Risk of lactic acidosis due to metformin may be increased secondary to hypoperfusion. In a scientific statement from the American Heart Association, metformin has been determined to be an agent that may exacerbate underlying myocardial dysfunction (magnitude: major) (AHA [Page 2016]). Use of metformin in patients with HF may be associated with reduced mortality and reduction in hospital readmission for HF (Crowley 2017; Eurich 2013).
- Hepatic impairment: The manufacturer recommends to generally avoid use in patients with hepatic impairment due to potential for lactic acidosis. However, continued use of metformin in patients with diabetes with liver dysfunction, including cirrhosis, may be associated with a survival benefit in carefully selected patients (Brackett 2010; Crowley 2017; Zhang 2014).
- Renal impairment: Metformin is substantially excreted by the kidney; assess renal function prior to initiation of therapy and periodically thereafter using eGFR. The risk of metformin accumulation and lactic acidosis increases with degree of renal impairment. Use of alogliptin/metformin combination product is not recommended in patients with eGFR 30 to 60 mL/minute/1.73 m2 and is contraindicated in patients with eGFR <30 mL/minute/1.73 m2. Use of concomitant medications that may affect renal function (ie, affect tubular secretion) may also affect metformin disposition. Metformin should be withheld in patients with dehydration and/or prerenal azotemia.
- Stress-related states: It may be necessary to discontinue metformin and administer insulin if the patient is exposed to stress (fever, trauma, infection, surgery).
Concurrent drug therapy issues:
- Drug-drug interactions: Potentially significant interactions may exist, requiring dose or frequency adjustment, additional monitoring, and/or selection of alternative therapy. Consult drug interactions database for more detailed information.
Special populations:
- Elderly: Use with caution; risk of metformin-associated lactic acidosis increases with age.
Other warnings/precautions:
- Appropriate use: Not for use in patients with diabetic ketoacidosis (DKA) or patients with type 1 diabetes mellitus.
- Ethanol use: Instruct patients to avoid excessive acute or chronic ethanol use; ethanol may potentiate metformin's effect on lactate metabolism.
- Iodinated contrast: According to the manufacturer, it is recommended to temporarily discontinue metformin at the time of or before iodinated contrast imaging procedures in patients with an eGFR 30 to 60 mL/minute/1.73 m2; or with a history of hepatic disease, alcoholism, or heart failure; or in patients who will receive intra-arterial iodinated contrast. Reevaluate eGFR 48 hours after imaging procedure; restart if renal function is stable. Alternatively, the American College of Radiology (ACR) guidelines recommend that metformin may be used prior to or following administration of iodinated contrast media in patients with no evidence of acute kidney injury (AKI) and with an eGFR ≥30 mL/minute/1.73 m2; ACR guidelines recommend temporary discontinuation of metformin in patients with known AKI or severe chronic kidney disease ([stage IV or V [ie, eGFR <30 mL/minute/1.73 m2]) or who are undergoing arterial catheter studies (ACR 2017).
- Patient education: Diabetes self-management education (DSME) is essential to maximize the effectiveness of therapy.
- Surgical procedures: Metformin should be withheld the day of surgery (all other oral hypoglycemic agents should be withheld the morning of surgery or procedure) (ADA 2019). Resume only after normal intake resumed and normal renal function is verified.
Monitoring Parameters
HbA1c (at least twice yearly in patients who have stable glycemic control and are meeting treatment goals; quarterly in patients not meeting treatment goals or with therapy change [ADA 2019]), serum glucose, hematologic parameters (eg, hemoglobin/hematocrit, red blood cell indices); hepatic function (prior to initiation of therapy and as clinically indicated thereafter), renal function (prior to initiation of therapy then annually or more frequent if necessary); vitamin B12 serum concentrations every 2 to 3 years; folate (if megaloblastic anemia is suspected); signs/symptoms of heart failure and pancreatitis.
Pregnancy
Pregnancy Considerations
Metformin crosses the placenta (ADA 2020). Refer to individual agents for additional information.
Patient Education
What is this drug used for?
- It is used to lower blood sugar in patients with high blood sugar (diabetes).
Frequently reported side effects of this drug
- Common cold symptoms
- Sore throat
- Stuffy nose
- Diarrhea
- Passing gas
- Nausea
- Vomiting
- Back pain
- Runny nose
Other side effects of this drug: Talk with your doctor right away if you have any of these signs of:
- Lactic acidosis like fast breathing, fast heartbeat, abnormal heartbeat, vomiting, drowsiness, shortness of breath, feeling very tired or weak, severe dizziness, feeling cold, or muscle pain or cramps
- Low blood sugar like dizziness, headache, fatigue, feeling weak, shaking, fast heartbeat, confusion, increased hunger, or sweating
- Heart problems like cough or shortness of breath that is new or worse, swelling of the ankles or legs, abnormal heartbeat, weight gain of more than five pounds in 24 hours, dizziness, or passing out
- Liver problems like dark urine, fatigue, lack of appetite, nausea, abdominal pain, light-colored stools, vomiting, or yellow skin
- Pancreatitis like severe abdominal pain, severe back pain, severe nausea, or vomiting
- Urinary tract infection like blood in your urine, burning or painful urination, passing a lot of urine, fever, lower abdominal pain, or pelvic pain
- Skin blisters
- Skin breakdown
- Severe headache
- Severe dizziness
- Passing out
- Vision changes
- Severe joint pain
- Persistent joint pain
- Stevens-Johnson syndrome/toxic epidermal necrolysis like red, swollen, blistered, or peeling skin (with or without fever); red or irritated eyes; or sores in mouth, throat, nose, or eyes
- Signs of a significant reaction like wheezing; chest tightness; fever; itching; bad cough; blue skin color; seizures; or swelling of face, lips, tongue, or throat.
Note: This is not a comprehensive list of all side effects. Talk to your doctor if you have questions.
Consumer Information Use and Disclaimer: This information should not be used to decide whether or not to take this medicine or any other medicine. Only the healthcare provider has the knowledge and training to decide which medicines are right for a specific patient. This information does not endorse any medicine as safe, effective, or approved for treating any patient or health condition. This is only a brief summary of general information about this medicine. It does NOT include all information about the possible uses, directions, warnings, precautions, interactions, adverse effects, or risks that may apply to this medicine. This information is not specific medical advice and does not replace information you receive from the healthcare provider. You must talk with the healthcare provider for complete information about the risks and benefits of using this medicine.